Integrative psychiatry goes beyond symptom management, offering a personalized approach that combines medication, nutrition, lifestyle changes, and therapy. It focuses on identifying and addressing root causes of mental health issues, such as nutrient deficiencies, hormonal imbalances, inflammation, or gut health problems. This method uses tools like functional lab testing, genetic analysis, and tailored care plans to improve mental well-being.
Here’s how it works:
- Initial Evaluation: A deep dive into your medical, psychiatric, and lifestyle history to uncover root causes.
- Functional Lab Testing: Identifies biological factors like nutrient deficiencies or gut imbalances.
- Personalized Plans: Combines medication, nutrition, exercise, and therapy to fit your needs.
- Ongoing Monitoring: Regular assessments ensure your plan evolves as needed.
This approach connects mental and physical health for long-lasting results, offering a more personalized path to mental wellness.
What Sets Integrative Psychiatry Apart
Combining Conventional and Alternative Therapies
Integrative psychiatry blends traditional Western approaches – like psychiatric medications and psychotherapy – with complementary therapies, such as herbal remedies, acupuncture, massage, biofeedback, and targeted supplements. This combination aims to create a more effective treatment strategy than relying on a single method alone.
“Integrative medicine combines conventional Western medicine with alternative approaches to care, such as herbal remedies, use of evidence-based supplements, acupuncture, massage, mindfulness, yoga, biofeedback, stress reduction techniques, and motivational interviewing.” – Robert M. McCarron, D.O., Professor of Psychiatry
A 2017 survey revealed that 33.2% of Americans already incorporate integrative health practices into their lives, including supplements, meditation, and chiropractic care. The market for integrative health and medicine was valued at $82.27 billion in 2020 and is projected to grow at an annual rate of 22% through 2028. This growth highlights a growing acknowledgment that mental health care is most effective when it addresses multiple aspects of well-being at once.
By combining these diverse tools, integrative psychiatry creates a foundation for addressing the root causes of mental health challenges.
Finding and Treating Root Causes
Unlike traditional psychiatry, which often centers on managing symptoms, integrative psychiatry focuses on uncovering the origins of those symptoms. This approach uses tools like functional lab testing to investigate biological factors such as inflammation, nutritional deficiencies, gut-brain axis imbalances, hormonal disruptions, and genetic variations.
“It is virtually impossible to find a medical or psychiatric cure if the pathogenesis for a disorder is unknown.” – Robert M. McCarron, D.O., Professor of Psychiatry
For example, research shows that exercise can reduce depression symptoms by 58%, compared to 22% in placebo groups. This underscores how targeting root causes – like how physical activity affects neurotransmitters and inflammation – can lead to significant improvements. Similarly, about 80% of patients experience insomnia during acute mental health episodes. Addressing sleep issues as a core problem, rather than treating them as side effects, is another hallmark of this approach.
Personalized and Whole-Person Care
What truly sets integrative psychiatry apart is its emphasis on tailoring care to the individual. It recognizes the deep connection between mental and physical health, along with factors like nutrition, sleep, stress, and lifestyle habits.
“Integrative medicine emphasizes treating the whole person – mind, body, and spirit – rather than just focusing on the disease or symptoms.” – Robert M. McCarron, D.O., Professor of Psychiatry
Treatment plans are not cookie-cutter. Instead, clinicians use frameworks such as IM-STEMS (Sleep, Trauma-informed care, Exercise, Mindfulness, and Supplements) to craft strategies that align with each patient’s unique needs. This collaborative approach ensures that factors like genetic makeup, biochemistry, lifestyle, and personal preferences are all considered. The result? A treatment plan designed specifically for you, addressing your body, mind, and circumstances.
sbb-itb-23f89d4
Introduction to Integrative Psychiatry
How Treatment Plans Are Created
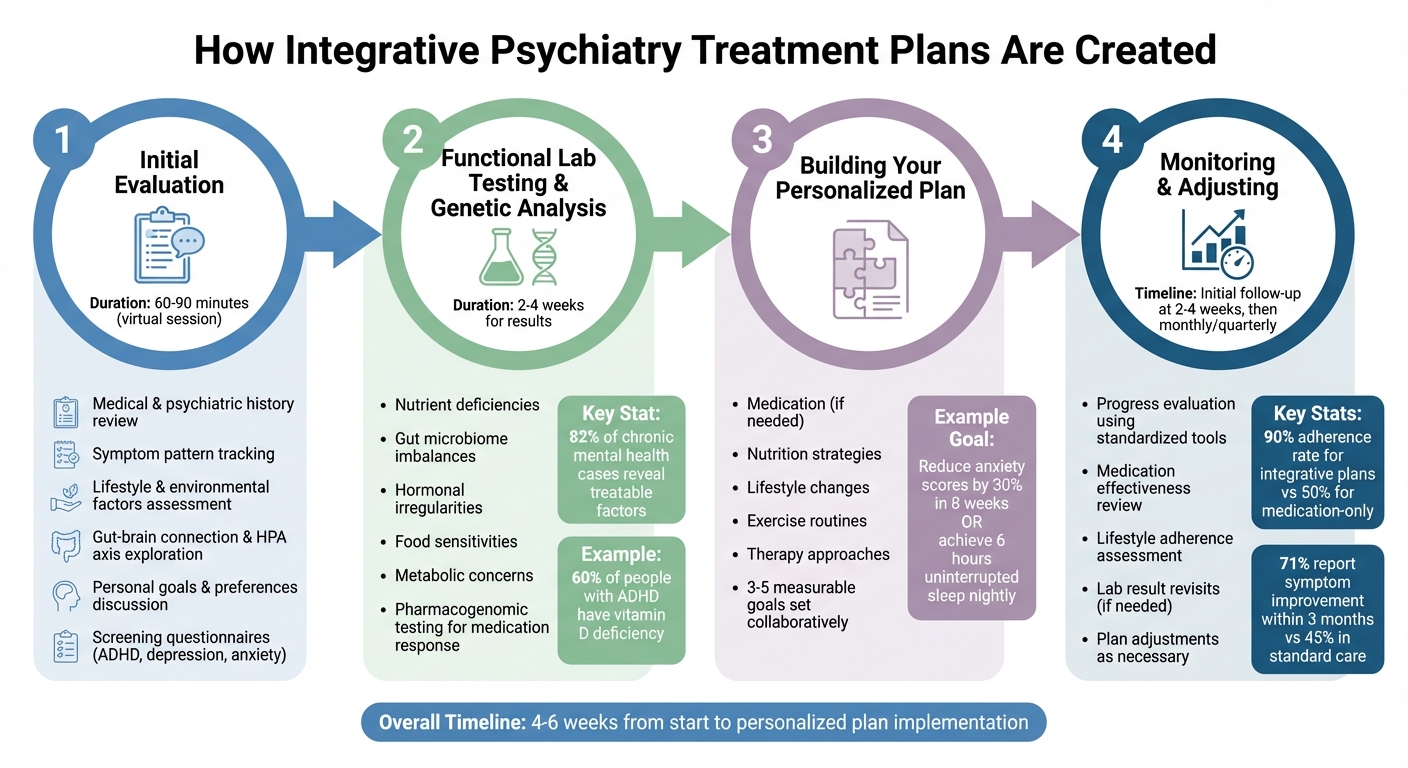
How Integrative Psychiatry Treatment Plans Work: 4-Step Process
Designing a psychiatry treatment plan is a collaborative effort that usually spans four to six weeks, though this timeline can shift depending on the complexity of your case and the types of testing involved.
Initial Evaluation
The process kicks off with a detailed evaluation that digs deeper than standard psychiatric assessments. During a 60–90 minute virtual session, your provider reviews your medical and psychiatric history, tracks symptom patterns, and examines lifestyle and environmental factors to uncover root causes. This includes exploring areas like the gut–brain connection and the HPA (hypothalamic-pituitary-adrenal) axis, which plays a role in the body’s stress response. Your personal goals and preferences are also discussed to ensure the approach aligns with your needs. Tools like ADHD, depression, or anxiety screening questionnaires may be used to assist in the evaluation.
“Root Cause Analysis is a cornerstone of the Modyfi Care Model in general, emphasizing the importance of identifying and addressing the underlying factors contributing to illness rather than merely alleviating symptoms.” – Modyfi Health
Following this in-depth session, your provider may recommend specific tests to better understand your unique imbalances.
Functional Lab Testing and Genetic Analysis
After the initial evaluation, functional lab tests may be ordered to identify biological issues that traditional psychiatry might overlook. These tests can reveal nutrient deficiencies, gut microbiome imbalances, hormonal irregularities, food sensitivities, and metabolic concerns. For instance, research shows that functional testing uncovers treatable factors in 82% of chronic mental health cases. A common example is vitamin D deficiency, which affects 60% of people with ADHD.
Pharmacogenomic testing is another key tool. It examines how your genetic makeup influences your response to medications, helping predict which psychiatric drugs and dosages might suit you best. This can reduce side effects and improve how well medications work.
The testing process typically takes two to four weeks, with results reviewed during a follow-up appointment. For convenience, lab kits can be shipped directly to your home for virtual care. These insights allow your provider to fine-tune every aspect of your treatment.
Building Your Personalized Plan
Once evaluations and testing are complete, your provider combines all the findings to create a tailored treatment plan. This plan may include a mix of medication, nutrition, lifestyle changes, exercise, and therapy, all customized to match your biology and goals.
For example, a 2022 Cleveland Clinic case study highlighted a 35-year-old woman with treatment-resistant depression. Her evaluation revealed low vitamin B12 levels and gut dysbiosis. Her plan included methylated B12 supplements, probiotics to restore gut health, and cognitive behavioral therapy. After six months of following the plan, her depression score (PHQ-9) dropped from 18 to 5. During this phase, you and your provider will work together to set three to five measurable goals, such as reducing anxiety scores by 30% in eight weeks or achieving six hours of uninterrupted sleep each night.
Once the plan is finalized, regular assessments ensure it evolves with your needs.
Monitoring and Adjusting Your Plan
After starting your personalized plan, your care team will closely monitor your progress. Initial follow-ups are usually scheduled two to four weeks after implementation, with monthly or quarterly check-ins depending on your progress and stability. These sessions evaluate improvements using standardized tools, review medication effectiveness, assess adherence to lifestyle changes, and, if needed, revisit lab results.
Research shows that integrative plans combining nutrition and lifestyle changes have a 90% adherence rate, compared to 50% for medication-only approaches (Journal of Clinical Psychiatry, 2022). Moreover, 71% of patients in functional psychiatry report noticeable symptom improvement within three months, compared to 45% in standard care (Institute for Functional Medicine, 2023).
If certain strategies aren’t working, your provider will adjust the plan. This could involve tweaking medication dosages, revising your nutrition plan, increasing therapy sessions, or introducing new lifestyle recommendations. Tools like real-time mood and food logs help your care team make timely adjustments.
Careful documentation of all changes ensures continuity, especially when multiple professionals like psychiatrists, nutritionists, and therapists are involved. This integrated approach helps ensure all elements of your treatment work together toward your shared goals.
What’s Included in Treatment Plans
Integrative psychiatry takes a multi-faceted approach to mental health, combining medication, nutrition, lifestyle changes, and therapy into a tailored plan that fits your individual needs. Each element plays a distinct role in supporting your mental well-being. Let’s break it down.
Medication Management
Medications are often a key part of treatment, but they’re not used in isolation. Instead, they’re paired with strategies like improved nutrition and exercise to maximize their effectiveness. Psychiatric medications, such as SSRIs, TCAs, or NDRIs, may be prescribed depending on your specific condition.
Why does this combined approach matter? Standard SSRI treatments show response rates of 40% to 60%, with remission rates only reaching 30% to 45%. By blending medication with other therapies, integrative plans aim to improve these numbers and provide better outcomes.
Nutrition and Lifestyle Strategies
Nutrition directly impacts mental health through the gut–brain axis. Licensed nutrition therapists design personalized plans based on your biological needs and lifestyle. These plans focus on key nutrients essential for mental health. For example:
- High zinc intake has been linked to a 28% lower risk of depression.
- Consuming about three cans of sugar-sweetened beverages daily increases depression risk by 25%.
“We approach nutrition as a cornerstone of mental health. Our licensed nutrition therapists help identify imbalances, support brain and gut health, and create individualized plans that align with your biology, lifestyle, and goals.” – Modyfi Health
Exercise is another critical piece. Movement specialists craft routines tailored to your needs, targeting mental health, hormone balance, and stress relief. Evidence backs this up: a meta-analysis of 24 studies with over 4,000 participants found that aerobic exercise was more effective at reducing depressive symptoms than standard depression care. Depending on your goals, your plan might include aerobic or high-intensity workouts to build resilience and regulate the HPA axis, the system that manages your stress response.
Additional lifestyle adjustments can also make a big difference. These might include:
- Light therapy to regulate your circadian rhythm.
- Meditation and mindfulness practices.
- Sleep optimization techniques.
- Sauna use for whole-body hyperthermia.
These interventions address underlying issues like inflammation and hormone imbalances. For instance, individuals with abdominal obesity face a 38% higher risk of depression compared to those with a lean BMI. That’s why managing weight through nutrition and exercise is often a focus.
Therapy and Emotional Support
Therapy is essential for emotional healing and self-discovery. It helps you explore how emotional stress interacts with physical systems like the HPA axis and gut–brain axis. Therapists work with you in three key areas: self-discovery, emotional regulation, and building deeper connections with yourself, others, and your environment.
This matters because genetics account for about one-third to one-half of depression risk. The rest comes from environmental and emotional factors, which therapy aims to address. Through techniques like mindfulness and boundary-setting, you’ll learn coping mechanisms that help you regain emotional control and build resilience.
Treatment often includes both individual therapy and group sessions. Individual sessions provide personalized care, while group therapy offers a sense of community and shared understanding. Together, these approaches create a solid foundation that complements other treatments like medication and nutrition therapy.
Integrative Psychiatry at Modyfi Health
Services Offered at Modyfi Health
Modyfi Health provides virtual integrative care to residents in Maryland, DC, Virginia, and Delaware, offering a range of services designed to address mental and physical health holistically. Initial psychiatric evaluations last 60 minutes, allowing providers to dive deeply into your history – covering mental health, physical health, lifestyle, and environmental factors. Follow-up sessions, tailored to your needs, typically range from 30 to 60 minutes.
Our network services can include:
- Medication management combined with pharmacogenomic testing (e.g., GeneSight®, Tempus®, Genomind®) to understand how your body processes psychiatric medications.
- Functional lab testing to evaluate nutrient levels, hormones, gut microbiome health, inflammation markers, and toxin exposure.
- Nutrition therapy, offering meal plans created by licensed nutritionists to support brain-gut health and regulate blood sugar.
- Personalized fitness routines crafted by exercise specialists.
- Evidence-based therapy for individuals and couples, using approaches like Emotionally Focused Therapy (EFT) and Gottman-informed methods .
- A unique “Formacist” service, helping patients navigate paperwork for FMLA, disability, and ADA accommodations.
This broad spectrum of services ensures care is customized to each individual’s needs.
How Modyfi Health Personalizes Your Care
Modyfi Health’s approach starts with a comprehensive evaluation that looks at your entire well-being. This method aligns with integrative psychiatry, focusing on root causes rather than just addressing symptoms. During your first appointment, providers work with you to identify underlying imbalances and then develop a treatment plan combining conventional medication with supportive therapies tailored to your goals.
“Our psychiatric providers take the time to understand the whole picture including mind, body, lifestyle, and environment.” – Modyfi Health
The clinic uses a multidisciplinary team of therapists, nutritionists, and exercise specialists to create a plan that fits your unique needs. This systems-based approach considers how interconnected areas, like the gut-brain connection or the hypothalamic-pituitary-adrenal (HPA) axis, influence overall health. For example, a teenager with ADHD might benefit from functional lab testing, meal planning, exercise therapy, and medication management. Meanwhile, an adult with depression could explore couples therapy, genetic testing for medication optimization, and lifestyle adjustments targeting gut health.
Benefits of Virtual Care
Modyfi Health’s virtual care model eliminates many traditional barriers to accessing care. Appointments are conducted on a secure, HIPAA-compliant telehealth platform, so there’s no need to travel. Just ensure you’re using a supported browser, have a stable internet connection, and are physically located in Maryland, DC, Virginia, or Delaware during your session.
In addition to video appointments, patients can message their providers through a secure app and use the “Front Desk” feature for online check-ins. The network accepts most major insurance plans and offers flexible payment options.
Conclusion
Integrative psychiatry takes a refreshing approach to mental health, focusing on you as a whole person rather than just a collection of symptoms. This method moves beyond generic treatment plans, emphasizing your unique needs and recognizing how factors like genetics, gut health, past experiences, lifestyle choices, and environmental influences shape your mental well-being. By addressing the root causes of mental health challenges, it aims to restore balance in your body, offering long-lasting improvements instead of short-term fixes.
What sets this approach apart is its focus on personalization. Your treatment plan is created in partnership with your provider, blending therapies like cognitive-behavioral therapy (CBT) with tailored strategies for nutrition, exercise, and medication. As one expert puts it, “The key is to recognize and honor individual preferences and comfort levels, ensuring that the chosen treatment aligns with the person’s values and goals”. This collaboration ensures that every step of your care reflects your personal values and priorities.
Another strength of this model is its systems-based perspective. It acknowledges that imbalances in one area, such as inflammation or gut health issues, can show up as anxiety, depression, or other mental health concerns. Tools like functional lab testing, personalized diets, and lifestyle adjustments work together to restore balance, addressing the underlying causes instead of just masking symptoms.
At Modyfi Health, we bring this personalized, systems-focused care directly to you through virtual services. This approach makes it easier than ever to access comprehensive care that supports every aspect of your well-being. By combining holistic principles with the convenience of virtual care, we ensure that treatment is not only effective but also accessible.
To complement your clinical care, practical tools like mindfulness techniques, breathing exercises, and dietary adjustments empower you to take control of your mental health. These strategies help you build resilience and maintain progress long after your sessions, putting you in the driver’s seat of your wellness journey.
Schedule your 60-90 minute initial evaluation with Modyfi Health to design your personal health blueprint.
FAQs
Who is integrative psychiatry best for?
Integrative psychiatry offers a personalized way to approach mental health, focusing on both relieving symptoms and addressing their root causes. It’s a great fit for those who want to blend traditional treatments – like medication and therapy – with complementary methods such as nutrition, exercise, and mindfulness practices. This approach is particularly effective for managing complex conditions like anxiety, depression, PTSD, or ADHD, while also emphasizing overall well-being and healthier lifestyle choices.
What lab or genetic tests might I need?
You might need blood tests to pinpoint biological factors that influence mental health, including mood, anxiety, or brain function. In some cases, genetic testing could also be suggested to determine how your body reacts to certain treatments. These tests are designed to help develop a care plan that’s specifically tailored to your individual needs.
How long until I notice improvements?
The time it takes to notice changes with integrative psychiatry depends on the person and their specific treatment plan. Some individuals might experience shifts in mood, better sleep, or reduced anxiety within 2 to 4 weeks. That said, achieving lasting results – such as those from lifestyle and nutritional changes – can take anywhere from 3 to 6 months. Staying patient and maintaining open communication with your provider is essential, as your care is customized to fit your individual needs.
