When your blood sugar fluctuates – either spiking too high or dropping too low – it can directly affect your mood and mental clarity. Research shows that unstable glucose levels can contribute to anxiety, irritability, sadness, and even depression. Here’s how it works:
- Low blood sugar (hypoglycemia) triggers stress hormones like cortisol and adrenaline, causing anxiety, shakiness, and irritability.
- High blood sugar (hyperglycemia) leads to brain inflammation and disrupts mood-regulating chemicals like serotonin and dopamine, resulting in fatigue and low mood.
- Blood sugar swings – common after high-carb meals – can worsen emotional stability and mental health over time.
Studies reveal that people with blood sugar imbalances, including those with diabetes, are at higher risk for mood disorders like depression and anxiety. Even non-diabetics can experience these effects if their glucose levels are unstable. Diet plays a major role, with high-glycemic foods linked to a Studies indicate that diets high on the glycemic index can significantly increase the risk of depression—in some cohorts by as much as 70%.
Key Takeaways:
- Your brain depends on steady glucose levels for mood regulation.
- Insulin resistance doubles the risk of depression.
- Blood sugar swings are a stronger predictor of anxiety and depression than static glucose levels.
Strategic Interventions like eating balanced meals (protein + healthy fats + fiber), avoiding high-glycemic foods, and staying active after eating can stabilize blood sugar and improve emotional well-being. Continuous glucose monitoring and functional lab testing can also help identify patterns and prevent further issues.
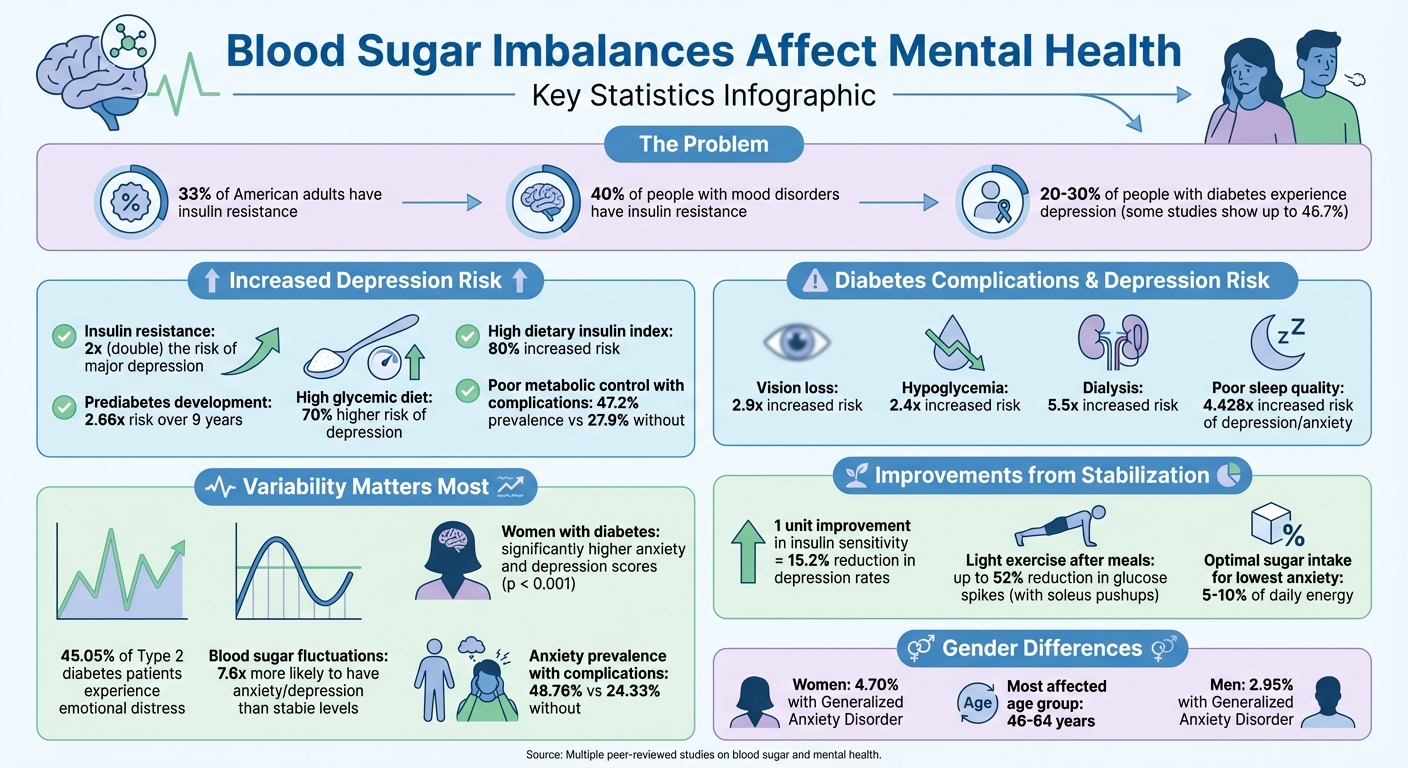
How Blood Sugar Levels Affect Mental Health and Mood Disorders
The Impact of Blood Sugar Levels on Mental Health: Understanding the Connection ✨
sbb-itb-23f89d4
How Blood Sugar Affects Mood: The Science
The relationship between blood sugar and mood is more complex than it might seem. It’s not just about energy dips or sugar highs – there are intricate connections involving hormones, neurotransmitters, and brain inflammation. These biological processes help explain why skipping meals can lead to anxiety or why sugary snacks might leave you feeling sluggish later.
Insulin and Glucose Regulation
Your brain relies on glucose as its primary energy source but lacks the ability to store it. When insulin resistance occurs – where cells stop responding effectively to insulin – excess sugar lingers in the bloodstream. This sugar can cross the blood-brain barrier, potentially harming brain tissue and disrupting critical functions.
Dr. Mehboob Ali Nazarani, a board-certified psychiatrist, highlights the importance of this process:
“It helps regulate neurotransmitters and inflammation in the brain, which are critical for stable mood and clear thinking.”
The statistics are striking. Roughly one-third of American adults have insulin resistance, and nearly 40% of those with mood disorders fall into this category. A 2021 study from Stanford University analyzed data from 601 participants and found that individuals who developed prediabetes within two years faced 2.66 times the risk of major depression over the next nine years compared to those with normal glucose levels. Dr. Natalie Rasgon, a professor at Stanford, summed it up:
“If you’re insulin-resistant, your risk of developing major depressive disorder is double that of someone who’s not insulin-resistant, even if you’ve never experienced depression before”.
This insulin imbalance doesn’t just affect energy – it sets off hormonal changes that can lead to mood swings.
Stress Hormones and Blood Sugar Changes
When your blood sugar drops, your body releases stress hormones like adrenaline, noradrenaline, and cortisol to restore glucose levels. While this helps replenish energy, it also has emotional consequences.
Timing plays a role here. After eating a high-glycemic meal, you may feel a temporary boost from dopamine, your brain’s “feel-good” chemical. But as insulin spikes and blood sugar crashes – typically four to five hours later – you might experience anxiety or irritability. This explains why a carb-heavy lunch can leave you feeling moody by mid-afternoon.
The relationship between stress and blood sugar is a two-way street. Chronic stress raises cortisol levels, which worsens insulin resistance. This creates a vicious cycle where unstable glucose levels and mood swings feed into each other. Skipping meals only adds to the problem, pushing your body into “starvation mode.” This high-stress state, marked by elevated cortisol and adrenaline, triggers catecholamine surges that result in reactive irritability—the biological root of the ‘hangry’ sensation.
Neurotransmitter Changes and Inflammation
Blood sugar fluctuations also disrupt neurotransmitter systems, particularly serotonin and dopamine, which are essential for mood regulation. Prolonged high glucose levels lead to increased inflammation and oxidative stress in the brain, further destabilizing these neurotransmitters.
The hypothalamus plays a key role here. AgRP neurons in this brain region signal the negative emotions associated with hunger. Once you eat and glucose levels normalize, these neurons quiet down, activating the brain’s reward system and shifting your mood from negative to positive. As Kristin Kaduk from the University of Tübingen explains:
“Hunger-related mood shifts depend on conscious sensing of the body’s internal state instead of acting subconsciously”.
Inflammation is another critical piece of the puzzle. Chronic high blood sugar and diets rich in refined carbohydrates promote inflammation, which significantly increases the risk of depression. Research shows that individuals with the highest dietary glycemic index are 70% more likely to develop Major Depressive Disorder, while those with a high dietary insulin index face an 80% increased risk. This underscores the strong connection between diet, inflammation, and mental health.
Research Findings: Blood Sugar and Mood Disorders
Recent research has taken a deeper dive into how blood sugar patterns influence mental health. The focus isn’t just on blood sugar levels themselves but also on the swings between those levels.
Low Blood Sugar and Anxiety Symptoms
A study published in Nutrition Journal involving 84,000 participants uncovered a U-shaped relationship between sugar consumption and anxiety. Both very low and very high sugar intakes were linked to increased anxiety symptoms. Interestingly, women seemed more affected by this pattern, with 4.70% experiencing Generalized Anxiety Disorder compared to 2.95% of men. The findings suggest that keeping sugar intake between 5% and 10% of daily energy needs is associated with the lowest risk of anxiety. While moderate sugar intake might slightly ease anxiety, excessive consumption does the opposite, amplifying symptoms.
Although low blood sugar contributes to heightened anxiety, high blood sugar takes a different toll, often triggering depressive symptoms.
High Blood Sugar and Depression Symptoms
Sustained high blood sugar, or hyperglycemia, has been strongly linked to depression. Chronic high glucose levels can lead to fatigue, low energy, and appetite changes, all of which contribute to a higher risk of depression. For individuals with obesity, improving insulin sensitivity by just one unit was associated with a 15.2% reduction in depression rates. Additionally, moderate-to-severe depression symptoms were found to correspond with a 6.7 mg/dl increase in glucose levels over time, highlighting a vicious cycle where poor mental health worsens blood sugar control.
Blood Sugar Fluctuations and Mental Health
It’s not just static blood sugar levels that matter – fluctuations between highs and lows appear to have a significant impact on mental health. Research published in BMC Endocrine Disorders followed 182 patients with Type 2 Diabetes and found that 45.05% experienced emotional distress. Those with greater blood sugar variability were 7.6 times more likely to suffer from anxiety and depression than those with stable levels. These fluctuations seem to be a stronger predictor of mood disorders than traditional markers like HbA1c or fasting glucose.
The effects of blood sugar swings are particularly noticeable in women and middle-aged adults (ages 46–64). Adding to the complexity, daily stress plays a role: studies using continuous glucose monitoring showed that stress significantly raises blood glucose levels in insulin-resistant individuals, with an increase measured at 6.24 × 10⁻³. One study summarized the relationship well:
“Blood glucose fluctuation and sleep quality are associated with the increased prevalence of depression and anxiety disorders in T2DM.”
Mood Disorders in People with Diabetes
When it comes to diabetes, the connection between blood sugar levels and mood swings becomes more pronounced. People with diabetes often face a higher risk of depression and anxiety, reinforcing the need for careful blood sugar management to support overall well-being.
Mental Health Challenges in Diabetes
Depression is a significant concern for individuals with diabetes, affecting anywhere from 20% to 30% of this population, with some studies reporting rates as high as 46.7%. In fact, people with diabetes are 1.33 times more likely to develop depression compared to those without the condition.
Diagnosing mood disorders in diabetes can be tricky because symptoms like fatigue and irritability overlap between the two. One of the most common depressive symptoms among diabetic patients is poor sleep quality, reported by 32.9% of individuals. This lack of restful sleep often stems from diabetes-related complications like peripheral neuropathy, which can cause chronic pain and disrupt sleep. Alarmingly, poor sleep quality increases the likelihood of experiencing depression and anxiety by over fourfold (4.428 times).
Complications related to diabetes can further destabilize mood. For instance, individuals with poor metabolic control and microvascular complications show a 47.2% prevalence of depressive symptoms, compared to 27.9% in those without such complications. Certain conditions, like vision loss (2.9x increased risk), hypoglycemia (2.4x increased risk), and dialysis (5.5x increased risk), significantly heighten the likelihood of depression. These findings underscore how physical health challenges in diabetes can intensify emotional struggles.
Gender Differences in Blood Sugar and Mood
Women with diabetes often face a heavier emotional toll compared to men. Studies reveal that women are more likely to experience anxiety, depression, and cognitive difficulties. Research measuring these symptoms found that women with Type 2 diabetes scored significantly higher on both the Self-rating Anxiety Scale and the Patient Health Questionnaire than men (p < 0.001).
Hormonal changes, particularly around menopause, may partly explain why women are more affected. These fluctuations can influence both blood sugar levels and emotional stability. Among diabetic patients dealing with complications, the prevalence of anxiety nearly doubles – 48.76% compared to 24.33% in those without complications – with women making up a larger share of those impacted.
How to Stabilize Blood Sugar for Better Mental Health
Improving blood sugar levels can have a direct impact on your mood and mental health. With a few targeted adjustments to your diet, health monitoring, and daily habits, you can make a noticeable difference.
Nutrition Therapy for Mood and Blood Sugar
What you eat – and how you eat it – plays a huge role in stabilizing blood sugar. A key tip? Pair carbohydrates with 20–30g of protein, healthy fats like olive oil or avocado, and fiber-rich vegetables. This combination slows down glucose absorption, helping you avoid those energy crashes that can wreak havoc on your mood.
Another helpful strategy is food sequencing. This means eating vegetables first, followed by proteins and fats, and saving carbohydrates for last. Studies show this approach significantly reduces post-meal glucose spikes compared to eating everything at once. Starting your day with a protein-packed breakfast – like eggs and spinach instead of sugary cereals – sets the tone for steady blood sugar and better mood throughout the day.
“Maintaining stable blood sugar levels isn’t just important for physical health – it plays a significant role in mental well-being. Rapid spikes and crashes in blood sugar can lead to mood swings, anxiety, brain fog, and even depressive symptoms.” – Staci Shacter, MS, RD, LDN, FHE Health
You can also tweak how you prepare your meals. Cooling cooked starches like potatoes, rice, and pasta before eating increases resistant starch, which supports gut health and helps reduce glucose spikes. Drinking a tablespoon of apple cider vinegar mixed with water before meals can temporarily slow down carbohydrate digestion. And sipping chamomile tea after meals may gradually improve insulin sensitivity. Even simple swaps, like choosing sourdough bread over regular bread, can make a difference.
These dietary habits set the stage for better understanding and managing your blood sugar patterns.
Monitoring and Functional Lab Testing
Standard glucose tests only scratch the surface. Functional lab testing – measuring HbA1c, fasting glucose, and fasting insulin – provides a more detailed look, revealing early signs of insulin resistance that could be impacting your mood. Catching this early can prevent it from escalating into diabetes while addressing mood swings and brain inflammation.
For continuous insights, Continuous Glucose Monitors (CGM) are a game-changer. These devices track blood sugar levels 24/7, helping you connect glucose spikes or crashes to feelings of anxiety, irritability, or even depression. For example, reactive hypoglycemia – when blood sugar dips below normal 4–5 hours after a high-carb meal – can trigger adrenaline and noradrenaline surges, leading to feelings of fear or aggression.
Modyfi Health integrates these advanced tools into personalized care plans. Their virtual clinic combines functional lab testing with psychiatric evaluations and therapy, addressing both blood sugar and mental health challenges from the ground up. Data is the antidote to guesswork. Schedule your evaluation to integrate CGM technology and functional testing into your personalized mental health blueprint.
Lifestyle Interventions
Beyond diet and testing, small lifestyle changes can help regulate blood sugar and improve your mental health.
Light exercise after meals – like a 10–15 minute walk or even light cleaning – encourages your muscles to absorb glucose, reducing blood sugar spikes. If walking isn’t an option, try simple movements like 10 air squats every 45 minutes or seated heel lifts (soleus pushups). These heel lifts alone can cut glucose spikes by up to 52%.
Sleep matters, too. Aim for 7–9 hours of quality sleep each night. Poor sleep worsens insulin resistance and increases cravings for sugary foods. And don’t underestimate the impact of stress – chronic stress raises cortisol levels, which can spike blood sugar and reduce insulin sensitivity. Incorporating relaxation techniques like deep breathing, yoga, or meditation can help counteract these effects.
Modyfi Health supports these lifestyle changes through telehealth services, offering exercise routines, sleep management tips, and stress reduction strategies. By combining functional testing with tailored lifestyle guidance, they help patients understand how specific meals or stressors influence their emotional well-being – empowering them to take control of their mental health.
Conclusion
The link between blood sugar levels and mental health is well-supported by scientific research. Fluctuations in glucose can trigger hormonal changes that disrupt mood, energy levels, and emotional stability.
“Understanding your blood sugar isn’t just about preventing diabetes – it’s about protecting your mental health, stabilizing your mood, and improving your quality of life.” – Mehboob Ali Nazarani, M.D., Board-Certified Psychiatrist
Fortunately, practical steps can help regulate blood sugar and, in turn, improve your mood. Simple strategies like pairing carbohydrates with protein, eating meals in a specific sequence, staying active after eating, and prioritizing sleep can have a noticeable impact on your daily well-being. For those managing depression, anxiety, or diabetes, addressing both mental and metabolic health is crucial. Ignoring the role of metabolic health in mood disorders leaves a key piece of the puzzle unresolved.
“Mental health treatment strategies should target every risk factor, including nutrition.” – The Conversation
An integrated approach that combines nutrition, lifestyle adjustments, and mental health care offers a more complete solution. Modyfi Health’s virtual clinic embodies this approach, offering services like psychiatric evaluations, functional lab testing, nutrition therapy, and lifestyle interventions. By addressing both physical and mental health together, you can step off the blood sugar-mood rollercoaster and take meaningful steps toward lasting well-being.
FAQs
How can I tell if my mood swings are from blood sugar?
Mood swings tied to blood sugar levels often follow noticeable patterns. You might feel irritable, anxious, or even “hangry”, particularly after eating or during periods of fasting. Other common signals include sudden energy crashes, intense cravings for sweets or carbs, brain fog, or unexplained fatigue. Both high and low blood sugar levels can affect your emotions, so keeping track of these symptoms and consulting a healthcare provider for testing can help identify the root cause.
What’s the best way to avoid a blood sugar crash after carbs?
To keep your blood sugar steady after eating carbs, combine them with protein, fiber, or healthy fats. These nutrients help slow down how quickly glucose enters your bloodstream, reducing the chances of sharp sugar spikes followed by crashes. Also, focus on balanced meals, stick to moderate portion sizes, and maintain a consistent intake of carbohydrates to support stable energy levels all day long.
Should I use a CGM or lab tests for mood-related glucose issues?
A continuous glucose monitor (CGM) offers real-time insights into blood sugar levels, making it easier to spot patterns that might connect to mood swings, such as anxiety or irritability. While lab tests are valuable for diagnosing conditions like insulin resistance or diabetes, they only provide a single moment-in-time measurement. For tracking daily blood sugar changes tied to mood, CGMs are more practical. On the other hand, lab tests are better suited for evaluating overall metabolic health.
