Functional medicine takes a different approach to treating depression and heart health by focusing on the shared biological causes of these conditions – like inflammation, hormonal imbalances, gut health, and nutrient deficiencies. This approach emphasizes addressing root causes rather than just managing symptoms. Key takeaways include:
- Depression and heart disease are closely connected: Nearly 44% of people with coronary artery disease also experience major depression. Both conditions share biological links, such as chronic inflammation and disruptions in stress-related systems.
- Inflammation is a major factor: Chronic low-grade inflammation contributes to both depressive symptoms and cardiovascular damage.
- Gut health matters: The gut-brain-heart axis shows how gut bacteria impact mood, stress response, and heart health.
- Personalized testing is critical: Functional medicine uses advanced diagnostics (e.g., hs-CRP, advanced lipid panels, hormone testing) to identify specific imbalances.
- Treatment focuses on lifestyle changes: Nutrition (e.g., Mediterranean diet), targeted supplements (e.g., omega-3s, magnesium), and stress management play a big role in improving both mental and cardiovascular health.
Functional Medicine Support for Depression and Mood Health
sbb-itb-23f89d4
Root Causes Linking Depression and Cardiovascular Health
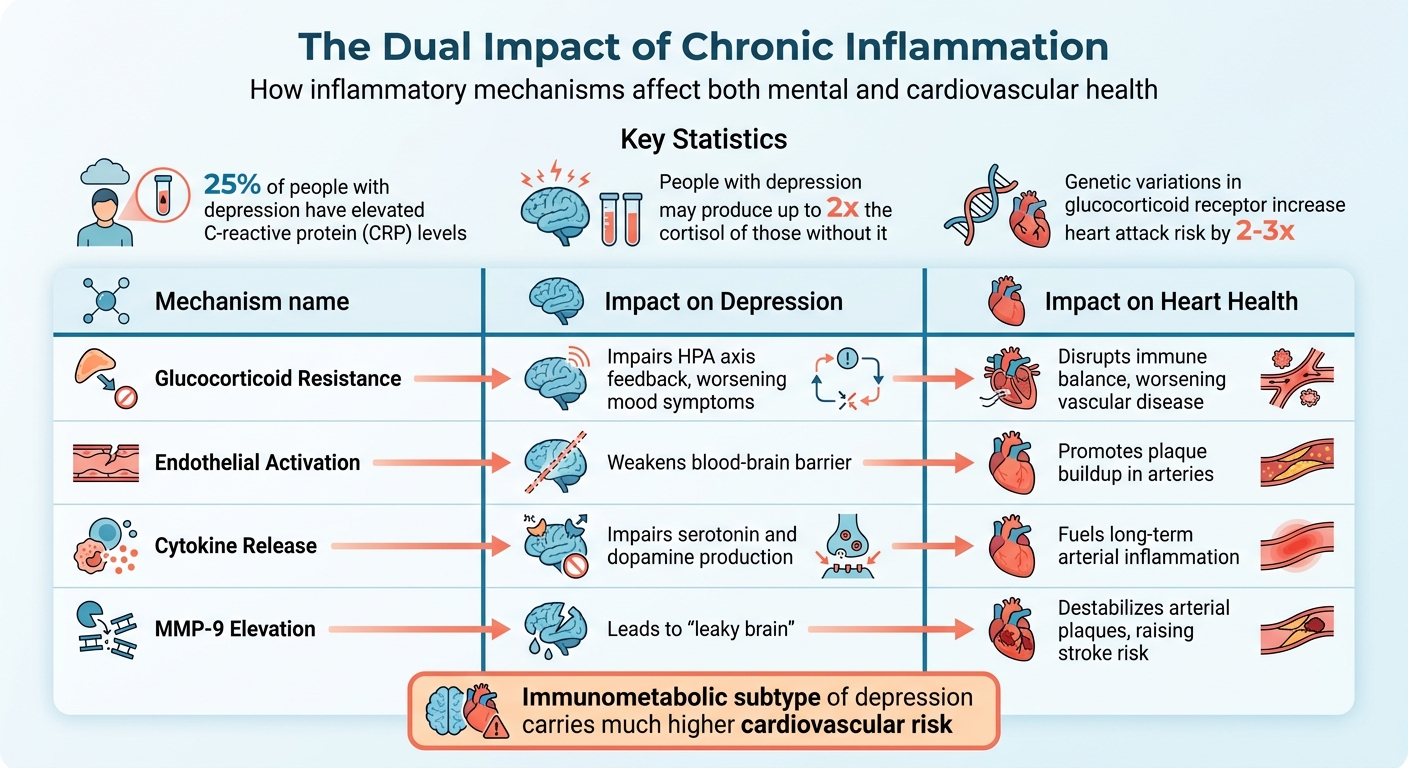
How Chronic Inflammation Affects Depression and Heart Health
Depression and heart disease are more intertwined than they might seem at first glance. Functional medicine digs into the shared biological mechanisms behind these conditions, which helps explain why treating just one often doesn’t lead to lasting results. By addressing these interconnected causes, a more tailored and holistic treatment approach becomes possible.
Chronic Inflammation and Its Dual Impact
Chronic, low-grade inflammation is a common thread linking depression and cardiovascular disease. For example, 25% of people with depression have elevated C-reactive protein (CRP) levels – a marker of systemic inflammation. This inflammatory state affects both the brain and the cardiovascular system in parallel.
“The neuroinflammatory hypothesis of depression… states that psychosocial stressors activate inflammatory responses causing release of pro-inflammatory cytokines and chemokines that contribute to monoaminergic and glutamatergic dysfunction.”
– BMC Immunology
When chronic stress disrupts the hypothalamic–pituitary–adrenal (HPA) axis, the body overproduces cortisol. Over time, tissues can become resistant to cortisol’s anti-inflammatory effects, a condition called glucocorticoid resistance. People with depression may produce up to twice the cortisol of those without it. This resistance allows inflammation to spiral out of control, leading to both depressive symptoms and vascular damage. Genetic variations in the glucocorticoid receptor can increase the risk of heart attack and coronary heart disease by two to three times.
Inflammation also activates endothelial cells in blood vessels, causing them to produce adhesion molecules like ICAM-1. This process not only drives atherosclerosis but also weakens the blood-brain barrier. ICAM-1 has been identified as a “hub gene” connecting depression to acute heart attacks. Additionally, the enzyme matrix metalloproteinase-9 (MMP-9), which is upregulated by inflammatory cytokines, damages tight junctions in the brain and destabilizes arterial plaques, increasing stroke risk.
| Mechanism | Impact on Depression | Impact on Heart Health |
|---|---|---|
| Glucocorticoid Resistance | Impairs HPA axis feedback, worsening mood symptoms | Disrupts immune balance, worsening vascular disease |
| Endothelial Activation | Weakens blood-brain barrier | Promotes plaque buildup in arteries |
| Cytokine Release | Impairs serotonin and dopamine production | Fuels long-term arterial inflammation |
| MMP-9 Elevation | Leads to “leaky brain” | Destabilizes arterial plaques, raising stroke risk |
Emerging studies also highlight an immunometabolic subtype of depression, driven by a mix of metabolic and inflammatory factors. This subtype carries a much higher cardiovascular risk compared to other forms of depression.
Hormonal and Nutritional Imbalances
Hormones and nutrients play a critical role in both mental health and heart function. Disruptions in sex hormones like testosterone, estrogen, or progesterone can throw off neurotransmitter systems, impacting serotonin and dopamine levels. These hormonal shifts also affect blood pressure and vascular health.
“Depression isn’t always caused by a neurotransmitter imbalance alone. For example, unregulated blood sugar can trigger fatigue and melancholy, while low thyroid function may cause brain fog and sluggishness.” Alternative Family Medicine & Chiropractic
Nutritional deficiencies compound these problems. Since nearly 90% of mood-regulating neurotransmitters are produced in the gut, nutrients like omega-3 fatty acids, magnesium, and vitamin D are essential for both brain and heart health. For instance, magnesium deficiency is linked to higher rates of depression and an increased risk of heart failure, while vitamin D helps regulate mood and protect the cardiovascular system.
Diet quality also matters. A higher Dietary Inflammatory Index (DII) – which measures how inflammatory a diet is – correlates with a 12.2% increase in the odds of congestive heart failure in people with depression. In older adults with depression, higher DII scores are tied to a greater likelihood of heart failure (odds ratio of 1.122).
“Inflammatory diets can increase pro-inflammatory cytokines, negatively affecting mood and potentially leading to depression. This inflammation also contributes to oxidative stress and endothelial dysfunction, raising cardiovascular risks.”
– Scientific Reports
Blood sugar imbalances also play a role. Fluctuating glucose levels can lead to mood swings and fatigue while increasing the risk of obesity, type 2 diabetes, and cardiovascular disease. Conditions like insulin resistance and hypothyroidism, often overlooked in standard tests, can strain both mental and physical health. These hormonal and nutritional issues also influence gut health and systemic inflammation, forming a bridge between the gut, brain, and heart.
The Gut-Brain-Heart Axis
The gut isn’t just about digestion – it acts as a control center for both mental and cardiovascular health. The gut–brain–heart axis is a communication network where gut microbes regulate immune responses, stress hormones, and inflammation. In a healthy gut, Firmicutes and Bacteroidetes make up about 90% of the microbial population.
When this balance is disrupted – a condition called dysbiosis – it can have widespread effects. Dysbiosis increases intestinal permeability, or “leaky gut”, allowing bacterial toxins like lipopolysaccharides (LPS) to enter the bloodstream. These toxins drive systemic inflammation, a key factor in both depression and atherosclerosis.
“The intestinal microbiota plays a crucial role in the neuroendocrine system and gut–brain axis. This system impacts the hypothalamic–pituitary–adrenal (HPA) axis to regulate your response to stressors, blood pressure, and vascular response.”
– Dr. Jennifer L. Weinberg MD, MPH, MBE
Gut microbes also produce metabolites that influence mood and heart health. Short-chain fatty acids (SCFAs) help regulate inflammation and support brain function, while trimethylamine N-oxide (TMAO) is linked to higher risks of heart failure and stroke. Additionally, neurotransmitters made in the gut – like serotonin and dopamine – not only affect mood but also play a role in heart rate and blood vessel tone.
Genetics further ties depression and cardiovascular disease together. For example, heart failure shares 92% of its genetic risk factors with major depressive disorder, while atrial fibrillation shares around 64%. These overlapping genetic factors highlight the importance of addressing gut health to improve outcomes for both mental and cardiovascular conditions. Functional diagnostic testing can help pinpoint these issues, enabling more effective, personalized treatments.
Functional Diagnostic Testing for Depression and Heart Health
Functional medicine uses advanced testing to pinpoint the biological imbalances that contribute to both depression and heart disease. It focuses on areas like inflammation, metabolism, hormones, and gut health.
Testing Protocols
Functional testing goes beyond standard screenings to uncover specific biochemical triggers. For example, high-sensitivity C-reactive protein (hs-CRP) measures low-grade inflammation, which can impact both blood vessels and brain function. The JUPITER trial found that lowering hs-CRP levels reduced cardiovascular events by 44%, even in individuals with normal LDL cholesterol levels.
Advanced lipid panels offer a deeper understanding of heart disease risk than traditional cholesterol tests. Interestingly, 50% of heart attacks occur in people with normal LDL cholesterol levels. Functional medicine practitioners often test for LDL particle number (LDL-P), Apolipoprotein B (ApoB), and Lipoprotein(a) [Lp(a)] to get a clearer picture. A triglyceride-to-HDL ratio above 3.0 (measured in mg/dL) is a warning sign of insulin resistance and metabolic issues.
“Roughly half of all heart attacks occur in people with normal LDL cholesterol levels. That statistic alone should prompt us to look deeper.”
– Holistic Health
Nutrient panels, such as NutrEval or SpectraCell, detect deficiencies in key nutrients like B vitamins, magnesium, zinc, and vitamin D. These are critical for neurotransmitter production and heart function. Over 20 nutrient deficiencies are linked to depression, and about 90% of individuals with obesity lack adequate vitamin D, which is essential for mood regulation. Standard magnesium tests can miss subtle deficiencies, so RBC magnesium testing is often used for more accuracy.
Metabolic markers like homocysteine play a dual role. Elevated homocysteine levels indicate vascular damage and B-vitamin deficiencies. A 5 μmol/L increase in homocysteine correlates with a 20–50% higher risk of coronary heart disease. Tests for fasting insulin and HbA1c help identify insulin resistance, which can affect both mood and cardiovascular health.
Gut microbiome analysis through stool tests like GI-MAP evaluates the gut-brain-heart axis. These tests identify issues like dysbiosis, intestinal inflammation, and elevated zonulin levels, which signal “leaky gut.” The gut’s health is closely tied to mood regulation.
“Nutrient deficiencies, hormonal imbalances, and neurotransmitter imbalances often result from gastrointestinal dysfunction.”
– Dr. Jaime Cloyd, ND
Hormonal assessments examine the HPA axis using four-point cortisol testing, thyroid function (TSH, free T3, free T4), and sex hormones (estrogen, testosterone, progesterone). The DUTCH Complete test provides insights into hormone metabolites and stress responses. Organic Acid Testing (OAT) is another tool that screens for imbalances in energy production, detoxification, and neurotransmitter metabolism through a simple urine sample.
“Organic acid testing (OAT) is an excellent starting point for specialty testing for MDD because it casts a wide net to screen for imbalances in energy production, neurotransmitter metabolism, detoxification, oxidative stress, and nutritional status.”
– Dr. Jaime Cloyd, ND
Other tests include the Omega-3 Index, which should fall between 8–12% for optimal anti-inflammatory benefits, and screening for obstructive sleep apnea in patients with depression and resistant hypertension. Sleep apnea can cause nighttime blood pressure spikes and damage to blood vessels.
These tests allow for customized treatments that address the root causes of both depression and cardiovascular issues.
Conventional vs. Functional Testing
Now, let’s compare functional diagnostics with conventional testing. Standard medical tests focus on diagnosing diseases based on symptoms. For example, psychiatric evaluations rely on DSM-5 criteria and tools like the PHQ-9, while cardiac assessments typically involve basic lipid panels, glucose tests, and blood pressure measurements. Unfortunately, these often overlook the underlying biochemical imbalances driving the conditions.
Functional testing, on the other hand, dives deeper. Instead of waiting for TSH levels to become severely abnormal, functional practitioners analyze free T3 and free T4 to catch thyroid issues early. Similarly, they measure ApoB or LDL-P to assess the number of harmful cholesterol particles, rather than relying solely on “normal” LDL cholesterol levels.
Here’s a side-by-side comparison:
| Feature | Conventional Testing | Functional Diagnostic Testing |
|---|---|---|
| Primary Goal | Rule out organic disease and diagnose based on symptoms | Identify root-cause imbalances and biochemical variations |
| Lipid Assessment | Total cholesterol, LDL-C, HDL, triglycerides | LDL-P, ApoB, Lp(a), LDL particle size |
| Inflammation | Standard CRP (if ordered at all) | hs-CRP, IL-6, Lp-PLA2, fibrinogen |
| Metabolic Markers | Fasting glucose, HbA1c | Fasting insulin, homocysteine, triglyceride-to-HDL ratio |
| Nutrient Analysis | Serum B12, iron, ferritin | RBC magnesium, Omega-3 Index, comprehensive micronutrient panels, OAT |
| Hormonal Assessment | Basic TSH, serum cortisol | Free T3, free T4, four-point cortisol, DUTCH Complete |
| Gut Health | Rarely tested unless severe GI symptoms present | Comprehensive stool analysis (GI-MAP), zonulin, microbiome diversity |
This deeper approach explains why 1 in 3 patients with major depressive disorder experience treatment-resistant depression. Conventional methods often miss the subtle dysfunctions in inflammation, metabolism, hormones, and gut health that functional testing aims to uncover. By addressing these factors, functional diagnostics pave the way for more tailored and effective treatments.
Personalized Treatment Strategies in Functional Medicine
Functional medicine takes a tailored approach to care, creating treatment plans that address inflammation, nutrient gaps, hormonal imbalances, and metabolic issues. By targeting the specific problems uncovered during testing, these strategies aim to improve both mood and cardiovascular health.
Nutrition and Dietary Interventions
The Mediterranean diet is widely regarded as a top choice for managing both mental and cardiovascular health. Packed with anti-inflammatory foods like fruits, vegetables, nuts, seeds, legumes, and seafood, this diet helps combat systemic inflammation, which can harm both brain cells and blood vessels.
Keeping blood sugar levels steady is another key focus. Cutting out refined sugars and processed carbs helps prevent blood sugar spikes, which are linked to mood swings and arterial stiffness. For instance, studies show that a 10% increase in ultra-processed food consumption raises depression risk by 11%. In fact, seven randomized controlled trials have confirmed that improving diet quality can significantly ease depressive symptoms, even without weight loss.
The connection between the gut, brain, and heart is also central to functional medicine. Feeding beneficial gut bacteria with fiber and polyphenols is a priority. Practitioners often recommend eating 24–30 different plant-based foods weekly to enhance gut microbiome diversity and reduce depressive symptoms.
Even small dietary changes can make a big difference
Eating 30 grams of nuts daily – roughly a small handful – has been shown to lower depression rates by 17%. Similarly, consuming fatty fish rich in EPA and DHA at least once a week supports both brain health and arterial function.
Functional practitioners often guide patients using the “Root Plate” method: fill half the plate with non-starchy vegetables, a quarter with fiber-rich carbs like legumes or quinoa, and the remaining quarter with quality protein such as salmon. Add 1–2 tablespoons of healthy fats, like olive oil or avocado, for balance. Specific anti-inflammatory foods like turmeric (curcumin), green tea, dark chocolate (at least 70% cocoa), walnuts, and berries are also recommended for their polyphenol content.
Take, for example, Jordan Sikes, a patient who followed a functional medicine program in October 2025. Under the care of Dr. Ann at Alternative Family Medicine & Chiropractic, Sikes addressed chronic back pain, depression, and anxiety through a personalized nutrition and movement plan. As a result, he lost 60 pounds and, under close clinical supervision, safely titrated off medications like Zoloft and painkillers as his systemic inflammation resolved.
“My quality of life is better now at 29 than it was at 20.”
Alongside these dietary changes, supplementation plays a key role in refining treatment plans.
Targeted Supplementation and Therapies
Functional medicine uses lab results to personalize nutrient protocols. Testing for deficiencies – like RBC magnesium, vitamin D, and omega-3 levels – ensures that supplements are dosed appropriately, avoiding both under-dosing and toxicity.
Different forms of magnesium are used for specific needs. For example, magnesium glycinate is ideal for improving mood and sleep, while magnesium oxide or citrate is better suited for addressing constipation. Similarly, vitamin D levels are carefully monitored to maintain optimal health without side effects.
| Supplement/Therapy | Target Outcome (Mental Health) | Target Outcome (Heart Health) |
|---|---|---|
| Omega-3 Fatty Acids | Supports mood and brain function | Lowers triglycerides and improves arteries |
| Magnesium | Reduces stress and improves sleep | Helps regulate blood pressure |
| Coenzyme Q10 (CoQ10) | Boosts energy and mitochondrial health | Supports heart cell energy |
| Vitamin D & K2 | Helps regulate mood | Promotes arterial flexibility |
| Curcumin | Lowers neuroinflammation | Reduces oxidative stress |
A functional mental health panel typically costs about $95 and includes tests for RBC magnesium, hs-CRP, OmegaCheck, vitamin D, and B12. More advanced tests can range from $200 to $2,000, while monthly supplement costs generally fall between $50 and $300.
Beyond supplements, advanced therapies like microcurrent neurofeedback can help regulate brain activity for anxiety and stress relief. Regenerative options, such as platelet-rich plasma (PRP), are used to reduce inflammation. Hormonal testing – covering testosterone, estrogen, progesterone, and cortisol – pinpoints imbalances that contribute to both depression and cardiovascular issues.
Cleveland Clinic researchers found that 31% of functional medicine patients improved their health scores by 5 or more points within six months, highlighting the effectiveness of these personalized strategies.
Lifestyle and Stress Management Techniques
Lifestyle changes are another vital component of functional medicine. Physical activity, for instance, is a cornerstone of treatment. Just a 30-minute walk can lower stress hormones and improve circulation. Regular exercise also enhances insulin sensitivity, reduces blood pressure, and boosts mood by releasing endorphins.
Stress management techniques like deep breathing, meditation, and mindfulness help calm the autonomic nervous system and reduce cortisol-driven damage to arteries. Sleep hygiene is also emphasized, as quality sleep lowers cortisol levels and protects blood vessel health.
Social connections and time spent in nature are integrated into care plans as well. Being in green spaces has been shown to reduce depressive symptoms and foster a sense of well-being. However, practitioners recognize the challenges patients face when making these changes. As Chad Balilo, MS, from UC Health, explains:
“The burden of all the changes a patient has to make can exacerbate depressive symptoms. For example, if food is central to how they interact with others and they can’t indulge in the same things, it can worsen the feeling of isolation.”
Functional medicine practitioners closely monitor metabolic health markers – such as weight, BMI, blood pressure, and fasting glucose – especially for patients on psychiatric medications that can affect metabolism. This ensures that interventions support both mental and cardiovascular health.
Treating depression early can significantly lower the risk of heart attacks
Research shows that treating depression early can significantly lower the risk of heart attacks or strokes. In fact, individuals with both depression and heart disease face higher mortality rates than those with just one condition. This underscores the importance of integrated care.
Modyfi Health’s virtual care model brings together these personalized strategies, offering services such as psychiatric evaluations, medication management, functional lab testing, nutrition therapy, meal planning, and exercise programs. By addressing the root causes of health issues, Modyfi Health provides comprehensive support for both mental and cardiovascular wellness.
Modyfi Health‘s Integrative Care Model
Modyfi Health operates as a virtual clinic, bringing functional medicine directly to patients in Maryland, DC, Virginia, and Delaware. By using a systems biology approach, the clinic combines psychiatric care, therapy, and nutrition services into a single, cohesive system. This method focuses on addressing the root causes of conditions like depression and cardiovascular issues, offering a range of services aimed at long-term health improvements.
Services Offered by Modyfi Health
Modyfi Health provides psychiatric evaluations that go beyond standard diagnostics, examining factors like nutrition, sleep, hormonal balance, and lifestyle alongside traditional methods. Functional lab testing plays a key role, identifying specific imbalances to guide personalized care plans for both mental and cardiovascular health.
Nutrition therapy targets biological factors affecting mood and heart health. Licensed nutritionists create meal plans designed to stabilize blood sugar, reduce inflammation, and support gut health – essential components for managing depression and maintaining cardiovascular well-being.
“Functional lab testing helps us identify root causes that traditional tests often miss… to uncover imbalances that may be contributing to anxiety, depression, fatigue, brain fog, or mood swings.”
Exercise therapy takes a tailored approach, offering more than generic fitness advice. Movement specialists design custom exercise plans that help regulate the nervous system and balance cortisol levels, enhancing both emotional and physical health.
“Exercise is more than physical movement, it’s the most powerful therapeutic tool we have to support emotional balance, cognitive function, and nervous system regulation.”
The clinic also offers individual and couples therapy, using evidence-based methods, and medication management that incorporates functional medicine principles alongside conventional psychiatric treatments. While Modyfi Health accepts most major insurance plans, it does not currently accept Medicare or Medicaid.
How Modyfi Health Supports Long-Term Outcomes
Modyfi Health’s personalized care doesn’t stop at diagnosis – it’s sustained through a multidisciplinary team. Psychiatrists, therapists, nutritionists, and exercise specialists work together to create unified treatment plans. These plans integrate dietary recommendations, medication, exercise routines, and lab results to ensure comprehensive care.
This approach aims to go beyond short-term symptom relief by addressing deeper issues like mitochondrial dysfunction, HPA axis imbalances, and chronic inflammation.
“Modyfi’s approach to psychiatry goes beyond medication management. We blend conventional diagnostics and medications with a root-cause lens to address nutrition, sleep, hormones, trauma, and lifestyle as part of your care.”
The virtual nature of Modyfi Health makes this care accessible without requiring in-person visits. Patients benefit from regular telehealth check-ins, lab monitoring, and personalized adjustments to their care plans. This ongoing support helps maintain adherence and achieve lasting results. According to the clinic, their model has shown 60-70% sustained remission rates for depression and 25-35% reductions in cardiovascular risk when patients follow personalized interventions for 6 to 12 months.
Conclusion
Functional medicine tackles the shared biological factors behind depression and cardiovascular issues by addressing chronic inflammation, hormonal imbalances, and gut health problems. Through personalized nutrition plans, targeted supplements, and lifestyle changes, it aims to enhance both mental and heart health.
A striking example comes from a Cleveland Clinic case study (January 2025). Janice Skeen, a 66-year-old battling heart failure, type 2 diabetes, and severe obesity, achieved remarkable results. Over 18 months on a whole-foods-based functional medicine program, she lost 130 pounds, demonstrated significant improvements in her kidney and liver function, and was able to carefully transition off insulin and heart medications under strict medical supervision, showcasing the potential of targeted metabolic restoration.
“By focusing on root causes rather than just symptoms, functional medicine can significantly improve cardiovascular outcomes.” – Dr. Kristin Robinson ND
This case highlights how addressing systemic imbalances can help reverse chronic conditions. Depression and heart disease are closely linked – elevated cortisol and inflammation from depression can harm the heart, while cardiovascular problems can worsen mental health. Functional medicine acknowledges this two-way connection and works to create lasting improvements by addressing the root causes of both.
FAQs
Can fixing inflammation improve both mood and heart risk?
Inflammation doesn’t just impact your body – it can influence your mind too. Chronic inflammation has been tied to serious conditions like depression and congestive heart failure. That means the effects go beyond physical symptoms, potentially affecting emotional well-being.
Functional medicine takes a different approach by systematically identifying and addressing the underlying root causes of inflammation. Through personalized care and tailored lifestyle changes, it aims to reduce inflammation, which may help support both cardiovascular health and mental wellness.
This holistic approach often involves adjustments in diet, stress management, and other daily habits to tackle inflammation from multiple angles.
Which labs best explain depression plus heart symptoms?
Labs that shed light on the connection between depression and heart symptoms often include advanced lipid panels. These tests measure markers like LDL particle number (LDL-P), ApoB, Lp(a), hs-CRP, and homocysteine. By offering a more detailed view of cardiovascular risk, they can reveal underlying factors that tie mental health to heart health. Functional medicine leverages this information to craft tailored care plans targeting both issues.
How long do diet and lifestyle changes take to help?
Diet and lifestyle changes can lead to noticeable benefits anywhere from a few weeks to a few months. The exact timeline varies from person to person and depends on the specific changes made. Staying consistent and tailoring adjustments to your individual needs are crucial for achieving results.
Ready to Transform Your Health From the Root Cause?
At Modyfi Health, we don’t treat symptoms in isolation. Our comprehensive virtual care model unifies expert psychiatric evaluations, advanced functional lab testing, targeted nutrition therapy, and personalized movement programs into a single cohesive system.
If you are ready to address the biological bridges between your mood, metabolism, and cardiovascular health, we are here to guide you.
👉 Schedule Your Comprehensive 60-Minute Evaluation Today
(Note: Modyfi proudly accepts most major insurance plans; currently, we do not accept Medicare or Medicaid.)
