Cortisol, often called the “stress hormone”, plays a key role in managing your sleep-wake cycle and stress response. Ideally, cortisol peaks in the morning to help you wake up and tapers off at night to support restful sleep. However, disruptions – like stress, poor habits, or irregular routines – can cause cortisol to spike at the wrong times, leading to sleep problems and health issues.
Key Takeaways:
- Cortisol’s Role: Regulates energy, alertness, and transitions between sleep and wakefulness.
- Disruptions: High cortisol at night can make it hard to fall or stay asleep and may cause early waking.
- Triggers for High Cortisol: Stress, late-night screen use, intense evening exercise, or poor diet.
- Impact of Sleep Loss: Increases cortisol levels, creating a cycle of stress and poor sleep.
- Solutions: Morning sunlight, consistent sleep schedules, calming activities, and balanced nutrition can help regulate cortisol.
Stress, Cortisol, & Sleep: An Awful Feedback Loop | Peter Attia, M.D. & Matthew Walker, Ph.D.
sbb-itb-23f89d4
How Cortisol Naturally Regulates Sleep
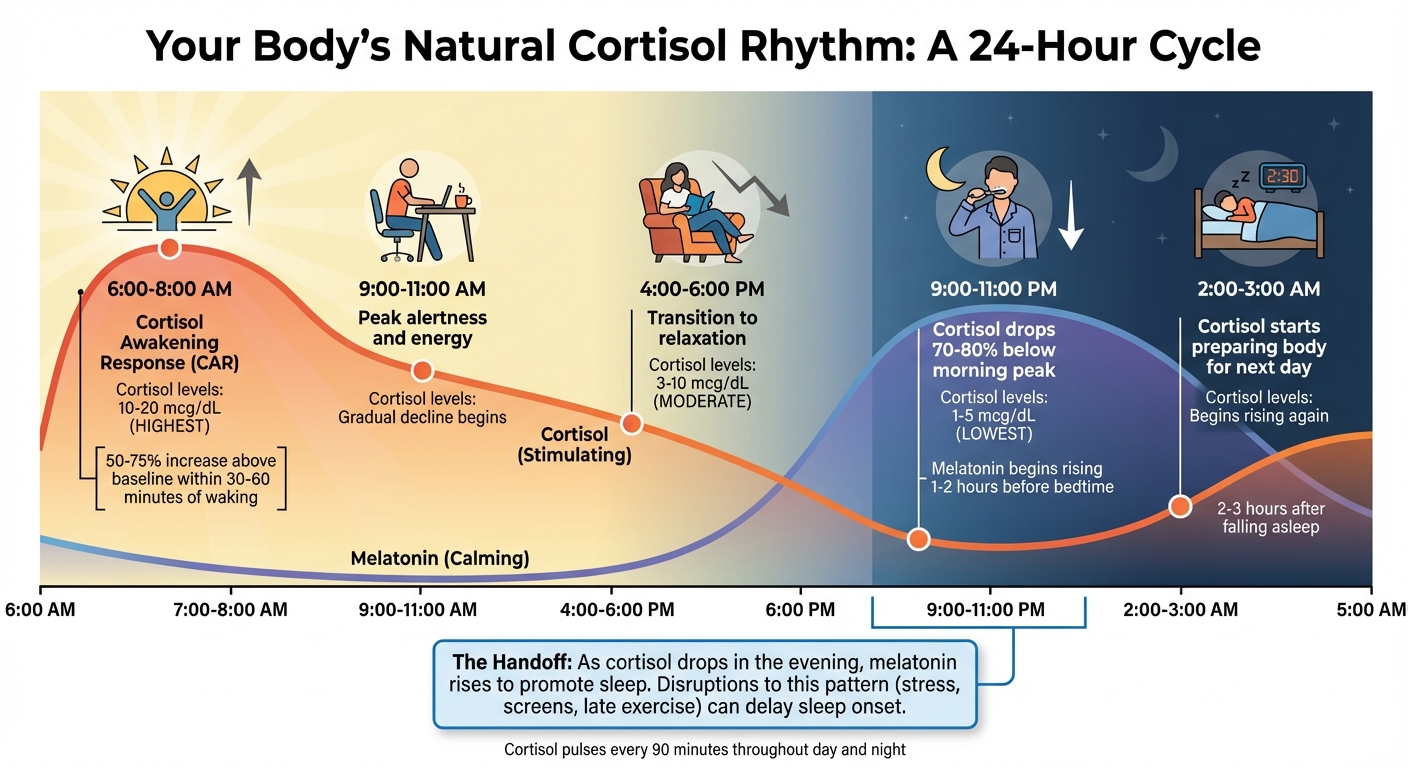
24-Hour Cortisol Rhythm and Sleep-Wake Cycle
The Daily Cortisol Pattern
Your body operates on a 24-hour internal clock, with cortisol playing a key role in keeping it on track. This rhythm is managed by the suprachiasmatic nucleus (SCN), a group of brain cells that uses light cues from your environment to maintain synchronization.
The day starts with the Cortisol Awakening Response (CAR), a sharp increase in cortisol levels 30–60 minutes after waking. During this time, cortisol can rise by 50–75% above baseline levels. This surge helps you wake up by boosting your heart rate, providing energy, and improving focus.
After the morning spike, cortisol levels gradually decline through the afternoon, transitioning your body from high alertness to a more relaxed state. By evening – typically between 9:00 p.m. and 11:00 p.m. – cortisol levels drop significantly, about 70–80% below the morning peak. This drop signals your body that it’s time to rest, paving the way for melatonin, the sleep hormone, to take over.
Interestingly, cortisol doesn’t remain static overnight. About 2–3 hours after you fall asleep, it starts to rise again, preparing your body for the next day. Additionally, cortisol pulses in shorter bursts approximately every 90 minutes throughout the day and night.
This predictable pattern plays a vital role in managing the transitions between being awake and asleep.
Cortisol’s Role in Sleep-Wake Cycles
Cortisol and melatonin work as opposites in regulating your sleep-wake cycle. As sleep expert Michael J. Breus, PhD, puts it:
“Cortisol is a stimulating, alerting hormone… stimulating wakefulness in the morning, continuing to support alertness throughout the day while gradually dropping to allow the body’s own internal sleep drive and other hormones to rise.”
When cortisol levels drop in the evening, they create the perfect conditions for melatonin to rise. Typically, melatonin begins increasing 1–2 hours before your usual bedtime, assuming cortisol has fallen sufficiently. This biological “handoff” ensures that cortisol steps back, allowing melatonin to take the lead.
Timing is everything here. Morning light exposure helps regulate your CAR, while dimming lights in the evening supports cortisol’s natural decline. On the flip side, late-night stress or exposure to bright screens can keep cortisol elevated, delaying melatonin production and making it harder to fall asleep.
How High Cortisol Disrupts Sleep
Interrupted Sleep and Shorter Sleep Duration
When cortisol doesn’t follow its natural nighttime decline, its persistent elevation acts like a built-in alarm system. This stress hormone keeps your nervous system on high alert, clashing with the calm state your body needs to drift into and maintain sleep.
Elevated cortisol at night disrupts both deep slow-wave sleep and REM sleep, which are critical for tissue repair, immune system support, emotional regulation, and memory processing. As researchers from IntraSleep explain:
“Stress hormones, primarily cortisol, can interfere with sleep architecture by increasing alertness and reducing deep and REM sleep phases, impairing memory, mood, and dream vividness.”
People with chronic insomnia often show significantly higher cortisol levels throughout the day, with the most noticeable spikes occurring in the evening – precisely when cortisol should be at its lowest. This creates a state of being “tired but wired”, where physical fatigue is paired with a heightened sense of alertness. Many individuals with elevated cortisol levels report waking up frequently around 3:00 a.m. or 4:00 a.m., as their cortisol begins to rise earlier than it should, disrupting the normal pre-dawn pattern.
Studies on Cushing’s syndrome, a condition marked by prolonged high cortisol levels, illustrate these effects clearly. Over half of patients with this condition experience insomnia and sleep disturbances, with 65.1% stating they “often or always” struggle to sleep. Additionally, research shows that even selectively suppressing slow-wave sleep – without reducing total sleep duration – can decrease glucose tolerance by about 25%.
Common Causes of High Evening Cortisol
Several factors can contribute to elevated cortisol levels at night, further disrupting sleep patterns. Psychological stressors, such as work-related pressures, relationship conflicts, or pre-sleep overthinking, can trigger the HPA axis, keeping cortisol levels elevated well into the evening.
Lifestyle habits also play a role. Eating refined sugars, high-fat foods, or salty snacks can stimulate cortisol production. Similarly, engaging in intense exercise late at night can cause a temporary cortisol surge, delaying sleep onset. During particularly stressful periods, cortisol levels can be up to 9 times higher than during calmer times.
Physical conditions like chronic pain and systemic inflammation can also elevate cortisol levels throughout the day and night. Hormonal changes, such as those experienced during menopause, may further disrupt cortisol regulation. Even one night of partial sleep deprivation can increase cortisol levels the following evening, delaying the natural drop in cortisol by over an hour. This creates a vicious cycle where poor sleep raises cortisol, which in turn makes it harder to sleep.
Recognizing these triggers is key to making lifestyle adjustments that can help rebalance cortisol levels and improve sleep quality.
The Two-Way Connection Between Sleep and Cortisol
How Sleep Loss Raises Cortisol Levels
Losing sleep sets off a cycle that feeds on itself: not getting enough sleep raises cortisol levels, and higher cortisol levels, in turn, can interfere with sleep patterns.
Even one night of poor sleep can push cortisol levels higher during the afternoon and evening – times when they should naturally be tapering off. A 2024 meta-analysis of 24 studies found that acute sleep deprivation led to an increase in serum cortisol levels (standardized mean difference [SMD] = 0.46). When cortisol was measured multiple times throughout the day, a steady rise was observed (SMD = 0.28). This lack of sleep not only raises baseline cortisol levels but also intensifies the body’s overall stress-response system, making the cortisol response to stress even stronger.
Dr. Michael J. Breus, a clinical psychologist and sleep expert, puts it this way:
“Poor, insufficient, irregular sleep increases the activity of [the HPA axis], leading to more stress, greater arousal, and over time to… health complications. And a more active HPA axis can interfere with the ability to maintain consistent sleep routines… It can be a vicious cycle.”
Over time, this heightened cortisol reactivity can disrupt its natural daily rhythm, throwing the body further off balance.
Flattened Cortisol Patterns and Health Risks
Chronic sleep problems can flatten the normal daily cortisol curve. Instead of peaking in the morning and declining at night, cortisol levels stay moderately elevated throughout the day, disrupting the body’s ability to suppress cortisol during deep sleep. This breakdown in rhythm interferes with the restorative deep sleep that’s essential for recovery and overall health.
A 2004 study in the Journal of Alternative and Complementary Medicine monitored 12 participants dealing with sleep and pain issues over eight weeks. Researchers Maurice Ghaly and Dale Teplitz collected saliva samples every four hours and found that participants initially had abnormal cortisol patterns. After treatment, their cortisol rhythms returned to normal – peaking in the morning and declining by evening. Participants also reported deeper sleep and lower stress levels, aligning with the objective data.
The risks of disrupted cortisol go beyond feeling tired. For example, limiting sleep to just 4 hours per night for six consecutive nights can result in glucose tolerance levels resembling early-stage type 2 diabetes, with glucose clearance slowing by 40%. Additionally, sleeping fewer than 7 hours per night increases the risk of developing type 2 diabetes by 9% for every hour of sleep lost.
How to Manage Cortisol for Better Sleep and Less Stress
Lifestyle Changes That Lower Cortisol
You can regulate cortisol by syncing your daily habits with your body’s natural rhythms. Start your day with 10–15 minutes of morning sunlight to activate your cortisol awakening response.
Stick to a consistent sleep schedule. Going to bed around 10:00 p.m. and waking at the same time every day helps align the HPA axis with your natural cortisol rhythm. Avoid intense exercise late at night, as it can elevate cortisol levels. Instead, choose calming activities like yoga or walking. Another helpful practice is cognitive offloading – spend 20–30 minutes in the early evening (at least 2 hours before bedtime) jotting down concerns or tasks. This can prevent bedtime overthinking and reduce cortisol spikes.
Breathing exercises, like the 4-7-8 technique (inhale for 4 counts, hold for 7, exhale for 8), can activate the vagus nerve, encouraging relaxation. A warm bath or shower 60–90 minutes before bed can also help you fall asleep faster by lowering your core body temperature.
Once you’ve made these lifestyle adjustments, testing your cortisol levels can provide a clearer picture of where additional support might be needed.
Testing Cortisol Levels and Personalized Treatment
Understanding your cortisol pattern allows for more precise solutions. Multi-point testing, which measures cortisol at different times of the day, provides a complete “cortisol curve” instead of a one-time snapshot. Typically, cortisol levels are highest in the morning (10–20 mcg/dL between 6:00–8:00 a.m.), drop to 3–10 mcg/dL in the afternoon (4:00–6:00 p.m.), and hit their lowest point in the evening (1–5 mcg/dL between 10:00 p.m.–12:00 a.m.).
A 2004 study in the Journal of Alternative and Complementary Medicine by Maurice Ghaly and Dale Teplitz monitored 12 participants with sleep and pain issues over eight weeks. By mapping their 24-hour cortisol profiles through saliva samples taken every four hours, researchers discovered abnormal patterns in participants. After treatment, their cortisol rhythms improved – nighttime levels dropped, and morning peaks aligned with the natural circadian rhythm. Participants also reported less pain and stress.
Modyfi Health uses functional lab testing to identify disruptions in cortisol rhythms and create customized care plans. This approach goes beyond generic sleep advice, addressing specific issues like elevated evening cortisol (which calls for relaxation strategies) or low morning cortisol (which might require support for the cortisol awakening response). Comprehensive testing often includes other biomarkers, such as hormones, nutrients, and inflammation markers, to design a plan tailored to your biology and lifestyle.
Dietary changes can also play a big role in balancing cortisol.
Diet and Supplements for Cortisol Balance
What you eat – and when you eat – has a direct effect on cortisol. Keeping blood sugar stable is key because cortisol and glucose are closely connected. Skipping meals or eating high-sugar foods can cause blood sugar crashes, leading to reactive cortisol spikes. Start your day with a high-protein breakfast that includes healthy fats and fiber within 60–90 minutes of waking. This supports the natural morning cortisol rise and helps avoid energy dips later in the morning.
For dinner, include 1/4 to 1/2 cup of slow-digesting carbs like quinoa or sweet potatoes. These help shift your body from cortisol to melatonin production by aiding tryptophan’s ability to cross the blood-brain barrier. Nutritionist Alissa Segersten explains:
“When evening nourishment is insufficient… the body may rely on cortisol to mobilize stored glycogen from the liver in order to keep blood sugar stable. This protective response can interrupt sleep.”
Incorporate magnesium-rich foods like spinach, avocados, dark chocolate, and pumpkin seeds to calm the nervous system and reduce neural excitability. Omega-3 fatty acids from sources like salmon, walnuts, and chia seeds can help lower inflammation and ease stress on the HPA axis. Adaptogens such as Ashwagandha and Rhodiola are known to reduce cortisol and improve stress tolerance. Additionally, Pantethine (a form of Vitamin B5) supports HPA axis communication and is often utilized in clinical protocols to support energy levels.
Dr. Yufang Lin from Cleveland Clinic highlights the importance of balance:
“Nutrition is absolutely important for coping with stress and supporting your mood, but there’s no single food that’s going to do it all.”
The goal is to create a nutrient-rich, anti-inflammatory eating pattern that works with your body’s natural cortisol rhythm instead of disrupting it.
Conclusion
Cortisol plays a crucial role in your body – it helps you wake up feeling refreshed and supports deep, restful sleep when it’s in sync with your natural rhythms. Problems arise when chronic stress, irregular routines, or poor sleep habits throw this balance off. If cortisol spikes at the wrong times or stays elevated into the evening, it can create a cycle where stress disrupts sleep, and lack of sleep worsens hormonal imbalances.
As Dr. Sarah Mitchell, a sleep and wellness researcher, explains, “Cortisol is the single most important hormone governing your sleep-wake cycle – and when it’s out of rhythm, no amount of sleep hygiene will fully compensate.” This highlights the importance of personalized testing and tailored solutions. The right approach to managing cortisol depends on whether the issue involves elevated evening levels, low morning peaks, or other disruptions.
The strategies we’ve covered – like getting morning sunlight, sticking to a consistent sleep schedule, eating a balanced diet, and practicing stress-reduction techniques – can help bring your cortisol levels back in line with your body’s natural rhythm. These changes not only support better sleep but also help reduce stress over time.
Modyfi Health provides functional lab testing and integrative care that goes beyond one-size-fits-all advice. Their team maps your cortisol curve to pinpoint specific issues, whether it’s high nighttime levels, low morning peaks, or an inverted rhythm. From there, they create a plan tailored to your needs, combining nutritional guidance, mental health support, and lifestyle adjustments to address the root causes of your sleep and stress challenges. If you are ready to move beyond symptoms and map your own biological rhythms, you can schedule a comprehensive evaluation here.
Balancing cortisol isn’t about being perfect – it’s about making thoughtful, consistent choices that promote better sleep, reduce stress, and improve your overall well-being.
FAQs
How can I tell if my cortisol is high at night?
High nighttime cortisol can show up in several ways, such as trouble falling asleep, waking up suddenly with a pounding heart, night sweats that aren’t linked to the room’s temperature, and feeling anxious during the night. These issues tend to be more frequent in women over 40. Keeping cortisol levels in check might help improve sleep and ease these nighttime disturbances.
What’s the fastest way to lower cortisol before bed?
The fastest way to bring down cortisol levels before bed is by practicing relaxation techniques like deep breathing, mindfulness, or gentle stretching. These methods help soothe your mind and ease stress. Tackling any worries or concerns earlier in the evening can also help you unwind and set the stage for better sleep.
When should I test cortisol, and what test is best?
Cortisol levels are typically highest in the morning, making it the ideal time for testing. Testing methods include blood, saliva, or urine samples. Among these, the four-point salivary cortisol test stands out for providing a detailed picture of your cortisol levels throughout the day. This method allows for a better understanding of your daily cortisol rhythm.
