Patient-centered goal setting in psychiatry focuses on aligning treatment with what matters most to you. Instead of just managing symptoms, this approach helps you work toward personal goals – like improving relationships, returning to work, or gaining independence. Studies suggest that alignment between patients and clinicians is associated with higher rates of goal attainment and improved outcomes. This method also boosts motivation, trust, and engagement in treatment.
Key takeaways:
- Higher success rates: Goal alignment improves outcomes in areas like employment and education.
- Increased engagement: Patients who set their own goals are more likely to stay committed to treatment.
- Better relationships: Collaborative goal setting strengthens trust between patients and clinicians.
- Effective tools: Techniques like Goal Attainment Scaling (GAS) and motivational interviewing help personalize and track progress.
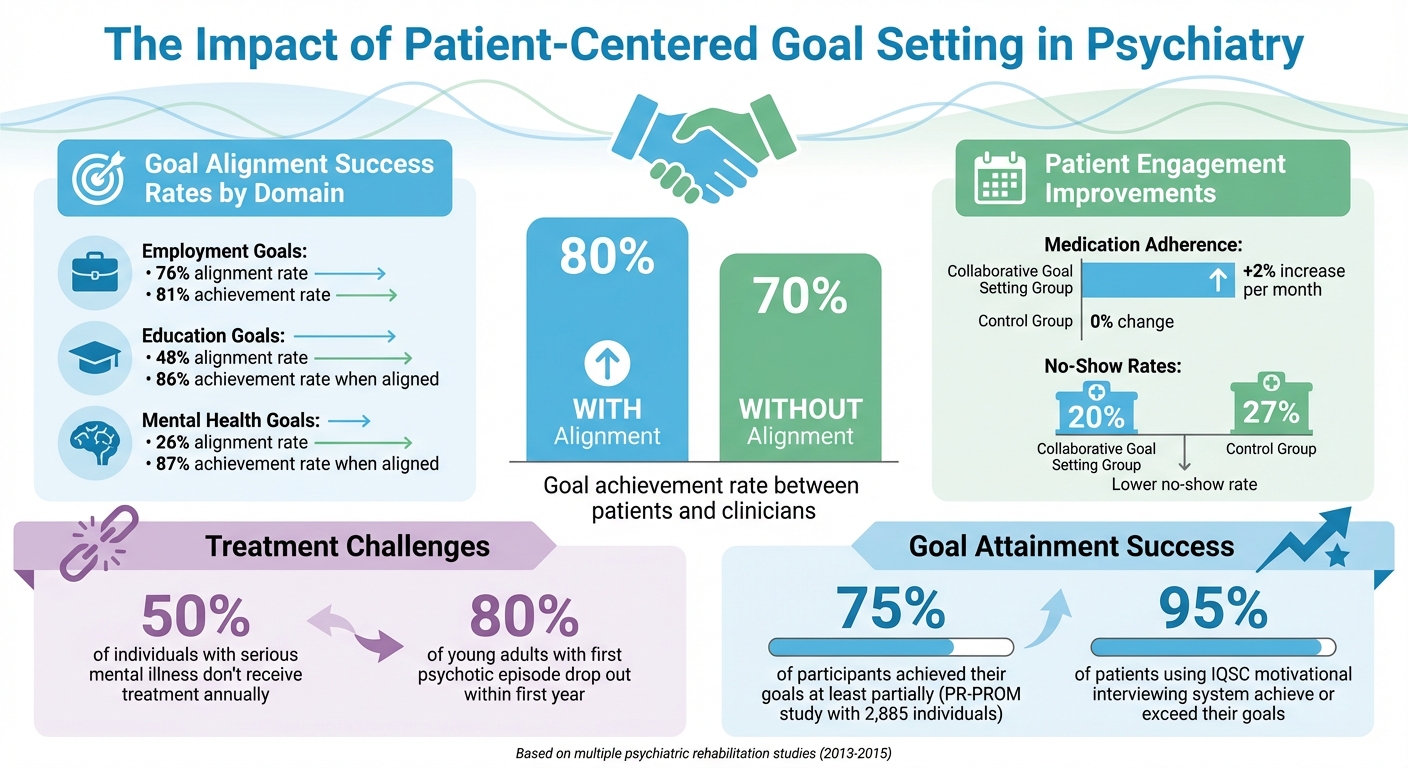
Patient-Centered Goal Setting Success Rates and Benefits in Psychiatry
Building a Person-Centered Plan Around a Meaningful Long-Term Goal Statement
sbb-itb-23f89d4
Benefits of Patient-Centered Goal Setting
Research consistently shows that personalized goal setting has a noticeable impact on treatment outcomes, patient satisfaction, and overall engagement.
Better Treatment Results
When patients and clinicians collaborate on setting specific goals, the outcomes are clear. A study conducted between April 2013 and April 2015 tracked 2,885 psychiatric rehabilitation participants across northern and central Israel using the Psychiatric Rehabilitation Patient Reported Outcome Measurement (PR-PROM). The findings revealed how alignment between patient and provider goals influenced success:
- Employment goals: 76% alignment and 81% achievement.
- Education goals: 48% alignment but an impressive 86% success rate when aligned.
- Mental health goals: Despite only 26% alignment, 87% success was achieved when there was agreement.
These results highlight how even modest alignment can lead to meaningful progress in mental health and life goals.
Higher Patient Satisfaction and Trust
Collaborative goal setting transforms the dynamic between patients and clinicians. A randomized controlled trial led by Victoria Stanhope, Ph.D., from May 2009 to March 2010, involved 367 clients across 10 U.S. Community Mental Health Centers. During the study, 84 providers were trained to identify life goals and document sessions collaboratively. Studies have shown improvements in medication adherence and reduced no-show rates with collaborative goal-setting interventions.
Dr. Stanhope emphasized the ethical importance of self-determination in mental health care, stating:
“Self-determination within mental health care has become an ethical imperative”.
By focusing on individual autonomy and fostering genuine collaboration, person-centered planning builds trust and strengthens the patient-provider relationship. This trust, in turn, encourages greater engagement, as discussed next.
Greater Engagement and Motivation
When patients are actively involved in setting their own goals, their motivation and commitment to treatment improve significantly. This approach connects with what truly matters to them – whether it’s returning to work, strengthening relationships, or managing daily responsibilities.
Engagement remains a critical challenge in mental health care. Studies show that up to 50% of individuals with serious mental illness don’t receive treatment annually, often due to a lack of connection or poor engagement. The issue is even more pronounced among young adults. Dropout rates in early psychosis can be very high, particularly among young adults, highlighting the importance of engagement-focused approaches. However, programs that emphasize individualized goals, such as education or employment, report higher retention rates.
Efrat Shadmi, Ph.D., from the University of Haifa, underscores the importance of this approach:
“Without a joint process of goal setting, consumers feel less motivated and are less likely to attain their goals”.
Research Studies on Goal Setting
The following studies highlight the impact of personalized goal setting across various psychiatric conditions, offering insights into its potential to improve patient outcomes.
GOALS Intervention for Bipolar Disorder
The Life Goals Collaborative Care (LGCC) program combines education on bipolar disorder with tailored goal-setting strategies. Conducted between 2002 and 2007, a study involving 164 outpatients compared the Life Goals Program to standard care. The program included six weekly sessions focusing on medication adherence and coping techniques. Participants who attended 4–6 sessions demonstrated improved attitudes toward medication at both 3 months (effect size 0.59) and 6 months (effect size 0.49).
A larger, three-year multisite trial revealed even more promising outcomes. Patients in the Life Goals intervention group experienced fewer weeks in affective episodes (p=.041) and showed significant reductions in social role dysfunction (p=.003) compared to those receiving usual care. This program also helps patients manage “reward sensitivity”, which minimizes extreme reactions to success and the pursuit of overly ambitious goals.
Jeffrey L. Susman, MD, highlighted a shift in treatment philosophy for bipolar disorder:
The goal of treatment for patients with bipolar disorder has changed in recent years from one of symptom abatement to one of recovery – that is, returning patients to their level of functioning prior to the onset of illness.
These findings suggest that personalized goal-setting programs like LGCC can significantly enhance recovery and functioning in bipolar disorder, paving the way for similar approaches in other psychiatric conditions.
Goal-Focused Supportive Contact (GFSC) for Schizophrenia
Between April 2013 and April 2015, the Israeli Psychiatric Rehabilitation Patient Reported Outcome Measurement (PR-PROM) project followed 2,885 individuals, 84% of whom had schizophrenia. Led by Efrat Shadmi, Ph.D., and David Roe, Ph.D., the study used Goal Attainment Scaling (GAS) to assess progress across various life areas.
Concordance rates varied by domain – 76% for employment, 71% for housing, but only 23% for family relationships and 15% for finances. Despite these variations, 75% of participants reported achieving their goals at least partially.
The study demonstrated that goals identified by patients were practical and age-appropriate, rather than influenced by psychosis. By using feedback tools to align patient and provider perspectives, recovery outcomes improved. These findings have since informed the application of personalized goal-setting methods in the treatment of major depressive disorder.
Goal Attainment Scaling in Major Depressive Disorder
Unlike traditional symptom-focused scales, Goal Attainment Scaling (GAS) emphasizes personalized, functional improvements – such as rebuilding relationships, maintaining a home, or regaining a sense of normalcy.
Research indicates that around 50% of patients with major depressive disorder (MDD) do not respond to first-line antidepressants. GAS offers a more nuanced measure of progress by focusing on goals that matter most to the individual. Despite this, surveys reveal that while most MDD patients have personal treatment goals, formal goal-setting is rarely incorporated into care plans.
Maggie McCue, from Takeda Pharmaceuticals, emphasized the relevance of GAS:
GAS is a relevant framework for setting personalized, meaningful treatment goals.
This approach is particularly valuable because it avoids “floor” and “ceiling” effects, which limit the sensitivity of traditional scales in detecting meaningful progress. By addressing individual priorities alongside symptom management, GAS aligns with the broader patient-centered approach of integrative psychiatry.
Methods for Implementing Goal Setting
Bringing patient-centered goal setting to life in psychiatric care requires practical methods that balance clinical expertise with what truly matters to patients. Three key approaches have gained traction: shared decision-making, motivational interviewing, and Goal Attainment Scaling.
Shared Decision-Making
Shared decision-making (SDM) is all about collaboration. Both patients and clinicians play an active role, sharing information and making treatment choices together. This method bridges the gap between a clinician’s focus on symptom relief and a patient’s desire for functional improvements – like better relationships, steady employment, or social engagement.
Patients can use “power statements” to clearly express their goals. A simple formula might look like this: “I want you to help me find a medication that will help me [symptom/function] so that I can [personal life goal]”. For example, 51% of patients using power statements cited improving social relationships as their top goal, while 19% prioritized employment.
However, challenges like power imbalances, doubts about patient capacity, and time constraints can hinder SDM. Still, research shows that when patients and providers agree on goals, the likelihood of achieving those goals increases by 70%. In fact, goal achievement rates jump to 80% when there’s alignment, compared to 70% when there isn’t.
Motivational Interviewing Techniques
Motivational interviewing (MI) helps patients clarify their goals and build the confidence to pursue them. The IQSC Framework is a four-step adaptation of MI principles designed for clinical use:
- Identify: Start by asking open-ended questions, like “What’s one habit you’re willing to change?”
- Quantify: Measure the current behavior to establish a baseline.
- Set: Agree on a goal the patient feels they can absolutely achieve.
- Confirm: Ensure the goal is truly theirs by offering an easier alternative. If they stick with their original goal, it shows ownership.
This method can help patients address the inner conflict of wanting change but fearing failure. Dr. Fox, Chief Medical Officer for CINQ Care, explained:
Too often, patients beat themselves up for failures and then give up, so it’s important to resolve ambivalence… When you resolve that ambivalence, guilt disappears and confidence improves.
Motivational interviewing has been shown to improve engagement, adherence, and goal attainment across a range of psychiatric conditions.
Goal Attainment Scaling (GAS)
Goal Attainment Scaling (GAS) offers a structured way to set and track personalized treatment goals. Unlike generic symptom checklists, GAS focuses on what truly matters to the patient – whether it’s returning to work, reconnecting with loved ones, or finding a sense of normalcy.
The system relies on SMART goals: Specific, Measurable, Attainable, Relevant, and Time-bound. Progress is measured on a five-point scale, ranging from –2 (baseline) to +2 (exceptional progress).
| GAS Score | Level of Attainment | Description |
|---|---|---|
| –2 | Baseline | The patient’s starting point before treatment |
| –1 | Less than expected | Some progress, but the goal wasn’t fully reached |
| 0 | Expected Outcome | The agreed SMART goal was achieved |
| +1 | More than expected | The patient exceeded the target |
| +2 | Much more than expected | Outstanding progress, far beyond the original goal |
The success of GAS depends on how well clinicians are trained to write and develop goals. A review of psychiatric goals found that while 70% included observable behaviors, only 7.8% were measurable. Training clinicians to focus on “approach” goals (moving toward something positive) rather than “avoidance” goals (moving away from something negative) can lead to better outcomes, especially for depression.
Maggie McCue from Takeda Pharmaceuticals highlighted the value of this method:
The goal attainment approach is a promising methodology that allows patients to work with their HCPs in setting individualized meaningful treatment goals.
GAS has been successfully applied in various psychiatric studies, including a phase 4 trial of vortioxetine for major depressive disorder and a 12-month study of donepezil hydrochloride in Alzheimer’s patients. By combining structure with personalization, GAS ensures that every goal is both meaningful and measurable.
Goal Setting in Integrative Psychiatry
Personalized and Root-Cause Focused Care
In integrative psychiatry, goal setting goes beyond addressing symptoms. Providers often ask, “What truly matters to you?”. This approach shifts the focus toward broader life ambitions, recognizing that symptom relief is often just a step toward achieving meaningful personal milestones – like maintaining a job, improving family relationships, or feeling more capable in everyday life.
Studies highlight the importance of aligning goals between patients and providers. When goals address crucial areas like physical health, work, and social connections, 80% of those goals are met. Compare that to a 70% success rate when such alignment is missing. This shared understanding transforms treatment into a collaborative journey, emphasizing a life of purpose rather than just ticking off clinical boxes.
This method builds on earlier practices, such as power statements, ensuring that treatment strategies align with what patients value most. Integrative psychiatry also incorporates digital tools to make care more accessible and tailored to individual needs.
Virtual Clinics and Accessibility
Virtual clinics, such as Modyfi Health, are breaking down barriers to personalized psychiatric care. For those who find in-person visits challenging – whether due to anxiety, transportation issues, or busy schedules – telehealth provides a convenient, stress-free option. Modyfi Health offers virtual integrative psychiatric services like medication management, therapy, nutrition counseling, and functional lab testing, all from the comfort of home.
Digital platforms also make setting and tracking SMART goals easier. In one study, 65.5% of patients reported sticking to the goals they set during their first counseling session. Virtual care ensures follow-up happens between appointments, keeping the goal-setting process dynamic and continuous. At Modyfi Health, personalized care plans combine mental health strategies, nutrition, and lifestyle adjustments to tackle root causes, helping patients work toward their aspirations.
Conclusion
Patient-centered goal setting transforms psychiatric care by focusing on achieving meaningful life outcomes rather than just managing symptoms. When patients and providers collaborate on specific goals – like maintaining a job, improving family connections, or gaining independence – treatment becomes a pathway toward the life patients envision for themselves.
The impact of this alignment is striking. When providers and patients are on the same page regarding goals, the success rate of achieving those goals jumps to 80%, compared to 70% when alignment is absent. This not only strengthens the therapeutic relationship but also enhances patient satisfaction and increases engagement in treatment efforts. Patients who take an active role in setting their own goals often experience greater motivation, improved quality of life, and a reduction in feelings of hopelessness.
Experts in the field emphasize the importance of this approach:
“Goal setting is at the heart of psychiatric rehabilitation and is a master signifier of the vision of recovery, because it translates into and motivates the process of creating a personally meaningful life.” – Efrat Shadmi, Ph.D.
Integrative care takes these benefits even further by addressing the patient as a whole person. By combining psychiatric treatment with physical health support, nutrition guidance, and lifestyle adjustments, integrative approaches create a more comprehensive care model. Virtual clinics, like Modyfi Health, illustrate how digital platforms can enhance access to personalized psychiatric care. These platforms seamlessly integrate services such as medication management, therapy, and nutrition counseling into unified care plans that address underlying challenges. They also make it easier to track progress between appointments, ensuring that goal setting remains flexible and responsive to a patient’s evolving needs.
FAQs
How do I choose goals that matter to me in psychiatry?
When setting goals in psychiatry, it’s important to focus on what truly matters to you. Think about areas in your life where you’d like to see progress – whether that’s strengthening relationships, managing symptoms effectively, or hitting personal milestones.
Work closely with your provider to create goals that are clear and realistic. Tools like motivational interviewing or the SMART framework (Specific, Measurable, Achievable, Relevant, Time-bound) can help shape these goals. By tailoring them to your values and priorities, you’ll find them more meaningful and easier to stick to, which can make a big difference in your mental health journey.
What if my clinician and I disagree on my treatment goals?
If you and your clinician have differing views on treatment goals, maintaining open communication is essential. Setting goals in psychiatric care works best as a collaborative effort, where respectful conversations help align your preferences with the clinician’s expertise. Regularly revisiting these goals and incorporating methods like motivational interviewing can bridge gaps in understanding. This approach encourages shared decision-making, helping to resolve disagreements constructively while improving both outcomes and overall satisfaction.
How is progress tracked with Goal Attainment Scaling (GAS)?
While more commonly used in research and rehabilitation settings, Goal Attainment Scaling (GAS) helps track progress by assessing the achievement of goals that are specific, measurable, attainable, relevant, and time-bound (SMART). Success is often gauged by the percentage of patients who achieve a GAS score of 50 or higher at a set follow-up point, such as week 12.
