Sleep is a cornerstone of children’s mental health. Poor sleep can lead to emotional instability, behavioral issues, and even long-term mental health conditions like anxiety, depression, and ADHD. At the same time, these conditions often make it harder for kids to sleep, creating a frustrating cycle.
Key takeaways:
- Emotional Regulation: Sleep, especially REM sleep, helps kids process emotions. Lack of it can lead to irritability, impulsivity, and difficulty managing feelings.
- Behavioral Challenges: Sleep-deprived children may exhibit hyperactivity, aggression, and trouble focusing, often mimicking ADHD symptoms.
- Mental Health Risks: Chronic sleep issues in childhood are linked to higher risks of anxiety and depression in adolescence and adulthood.
- Consistency Matters: Irregular sleep schedules disrupt emotional control, even if total sleep hours are adequate.
Practical steps to improve sleep include maintaining consistent bedtimes, creating calming bedtime routines, limiting screen time before bed, and addressing potential sleep disorders with professional help.
Sleep is not just rest – it’s a vital part of mental and emotional well-being.
The Truth About Child & Teen Sleep Deprivation
sbb-itb-23f89d4
How Poor Sleep Disrupts Emotional and Behavioral Control
When kids don’t get enough quality sleep, it can quickly throw off their ability to manage emotions and behaviors. Sleep plays a key role in helping children regulate their feelings and reactions. Without proper rest, this system falters, leading to noticeable challenges.
Sleep’s Impact on Emotional Stability
Sleep and mood are deeply interconnected. In fact, they influence each other in both directions. A study conducted in February 2024 by Jennifer M. Meigs and her team at the National Institute of Mental Health explored this link in 125 children and teens aged 8–18. Using digital surveys completed three times daily over seven days, they found that less sleep was tied to higher irritability in the morning (b ≤ −.09, p < .049). For children with conditions like ADHD and DMDD, parents reported that evening anger often led to shorter sleep durations that night (b = −.17, p = .019).
“It’s becoming increasingly clear that sleep and mood have a bidirectional relationship”.
Andrea Goldstein-Piekarski, PhD, from Stanford Medicine, explains that poor sleep weakens emotional control, which in turn can make it tougher to fall asleep the next night. This creates a frustrating cycle. Younger children are especially affected, and the problem is even worse for kids who already struggle with irritability.
Behavioral Problems Caused by Sleep Deprivation
The effects of poor sleep go beyond just feeling cranky. Sleep-deprived kids often show more serious behavioral issues like aggression (both physical and verbal), trouble focusing, daytime drowsiness, and struggles in school. These behaviors are not just a result of being tired – they stem from disrupted emotional regulation.
Chronic sleep problems can have long-term consequences. Kids with insomnia are 17 times more likely to develop anxiety and 10 times more likely to experience depression compared to their well-rested peers. Among children diagnosed with depressive disorders, an alarming 72.7% also reported sleep disturbances. Regularly missing out on sleep increases the risk of aggressive behavior, anxiety, and depression, which can carry over into adulthood.
These findings emphasize the importance of addressing sleep issues early. The next section will explore practical ways to help children get the rest they need.
Sleep and Specific Mental Health Conditions
Poor sleep doesn’t just affect mood or energy levels – it can deeply influence specific mental health conditions in children. By understanding these connections, parents and caregivers can better identify when sleep issues might be compounding other challenges.
How Sleep Affects ADHD Symptoms
The link between sleep and ADHD is especially intricate. Studies estimate that over half of children with ADHD face significant sleep disturbances, with some findings pushing that number as high as 75%. Lack of sleep can make ADHD symptoms like hyperactivity, impulsivity, and trouble focusing even worse.
Dr. William Benson, a psychologist at the Child Mind Institute, highlights the difficulty these children face:
“Being able to wind down, calm your thoughts, and settle your body is a form of self-regulation. And that’s something kids with ADHD struggle with.”
In many cases, children with ADHD may resist bedtime routines, take longer to fall asleep, or engage in activities that overstimulate them before bed, which frequently compounds their daytime challenges. Adding to the problem, medications like Ritalin or Adderall can delay sleep onset, creating a cycle of sleep deprivation.
Biologically, ADHD and sleep disorders share some common ground, including neurotransmitter imbalances and differences in the prefrontal cortex. Children with ADHD also tend to get less slow-wave deep sleep (important for physical recovery) and REM sleep (key for emotional regulation). Interestingly, research suggests that insufficient sleep during early childhood might even increase the risk of developing ADHD later in life.
Sleep’s Connection to Anxiety and Depression
Sleep plays a major role in mood disorders like anxiety and depression. Among children with depressive disorders, sleep problems are widespread: 53.5% experience insomnia, 9% deal with hypersomnia (oversleeping), and 10% struggle with both. Epidemiological studies suggest that chronic insomnia can significantly elevate the risk of depression and anxiety compared to the general population
For children with anxiety, nighttime can be especially challenging. Worry often triggers a cortisol spike, making it hard to relax and fall asleep. Depression-related sleep issues, on the other hand, often include waking up too early and being unable to fall back asleep, hypersomnia, or frequent nightmares.
Teenagers face an added challenge: during puberty, their melatonin production naturally shifts later by about two hours. Combine that with anxiety or depression, and it’s no surprise that up to 80% of teens don’t get enough sleep. This lack of rest can worsen mental health symptoms, creating a vicious cycle of sleep debt and emotional struggles.
Sleep apnea is another factor to consider. This condition, which disrupts breathing during sleep, triples the risk of anxiety and depression. Poor sleep not only intensifies these issues but also makes it harder for children to regulate their emotions and behavior.
Recognizing these connections is the first step toward finding practical ways to improve children’s sleep and, in turn, their mental health.
Practical Ways to Improve Children’s Sleep
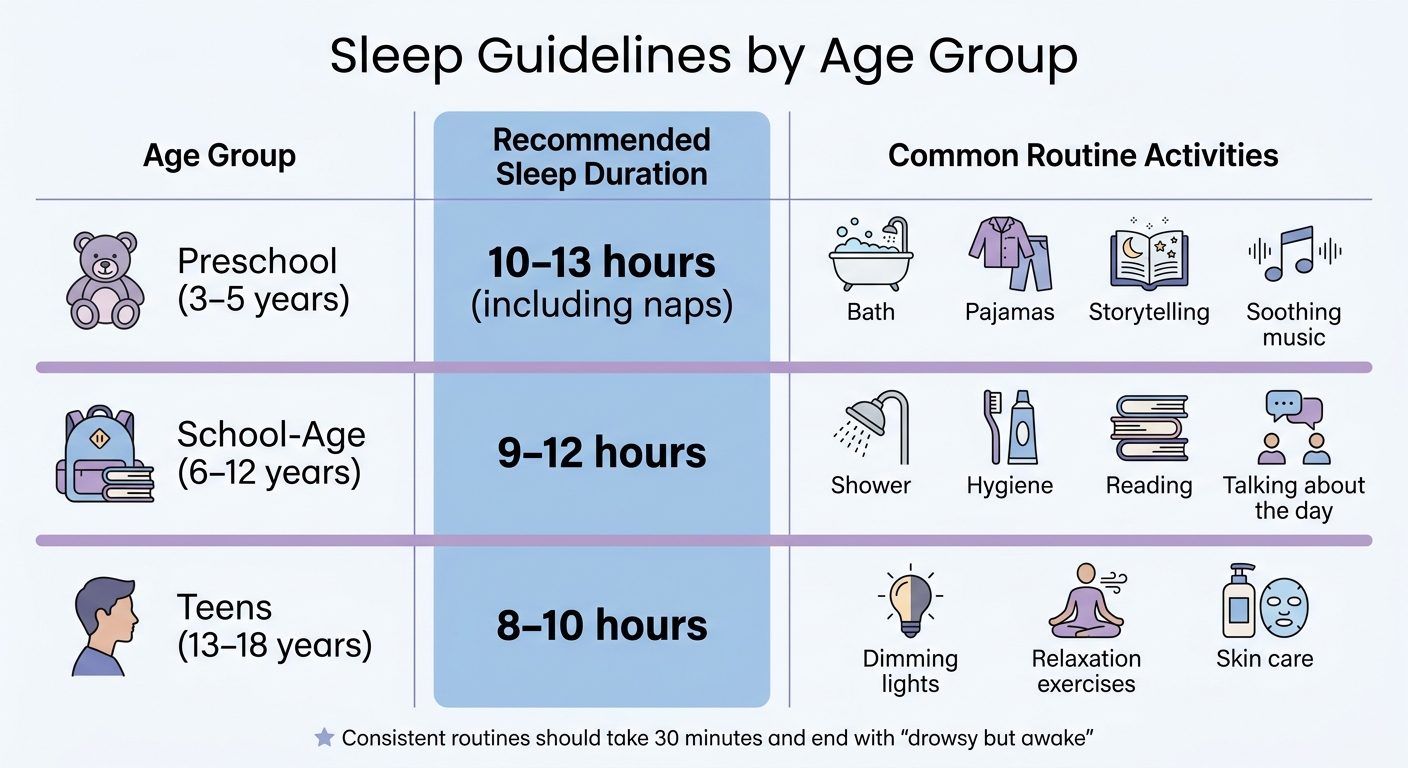
Recommended Sleep Duration by Age Group for Children’s Mental Health
You don’t need fancy gadgets or drastic lifestyle overhauls to help your child sleep better. By focusing on routines and creating the right environment, you can see noticeable improvements in just two weeks. Better sleep not only boosts emotional regulation but also supports healthier behavior and mental well-being.
Building Consistent Sleep Routines
A predictable bedtime routine is a game-changer. It should include three to four calming activities done in the same order every night – like taking a bath, brushing teeth, reading a story, or listening to relaxing music. Danielle Pacheco from the Sleep Foundation describes the purpose of these routines:
“Bedtime routines are a consistent, repetitive set of activities that are carried out before bed every night. They help prepare your child for sleep by having them relax and wind down”.
Keep the routine short – about 30 minutes, or a bit longer if it includes a bath. The goal is the “drowsy but awake” method: put your child to bed when they’re sleepy but still awake. This teaches them to self-soothe and fall asleep on their own, reducing nighttime awakenings.
Be mindful of screen time. Screens should be off at least an hour before bed. Blue light disrupts melatonin production, making it harder for kids to unwind. During the day, encourage physical activity and some sunlight exposure, especially in the morning, to help regulate their internal clock. Also, keep wake-up and bedtime consistent – even on weekends. Sleeping in more than an hour can mess up their sleep schedule for the week ahead.
| Age Group | Recommended Sleep Duration | Common Routine Activities |
|---|---|---|
| Preschool (3–5 years) | 10–13 hours (including naps) | Bath, pajamas, storytelling, soothing music |
| School-Age (6–12 years) | 9–12 hours | Shower, hygiene, reading, talking about the day |
| Teens (13–18 years) | 8–10 hours | Dimming lights, relaxation exercises, skin care |
Pairing a consistent routine with a well-prepared sleep environment makes a big difference.
Setting Up a Better Sleep Environment
The bedroom should be a calm, sleep-friendly space. Keep it cool, dark, and quiet. A white noise machine or fan can help block out household noise, and if your child is afraid of the dark, a dim, warm-colored nightlight works well. Dr. Elana Pearl Ben-Joseph advises:
“The bed is a place to feel relaxed and sleepy, not a place for tossing and turning”.
Gina McDowell from the Kids Mental Health Foundation adds:
“Ideally, kids should be in bed only when they are sleeping and not when they are watching TV, on their phone, doing schoolwork, eating, or doing any other activity”.
For younger children, a comfort item like a stuffed animal or a favorite blanket can help them feel secure and fall asleep more easily.
Watch out for caffeine. Avoid it after 3:00 p.m., and don’t forget about hidden sources like chocolate, certain sodas, or even some breakfast cereals. If your child naps, keep naps short – 20–30 minutes – and schedule them at least four hours before bedtime to ensure they’re ready to sleep at night.
Treating Sleep Disorders
If these strategies don’t help after two weeks, it’s time to consult a pediatrician. Persistent issues like trouble falling asleep, frequent waking, snoring, or breathing pauses during sleep might signal a deeper problem. Dr. Vaishal Shah from Cleveland Clinic highlights:
“Sleep is important for many aspects in health. Our attention span and memory learning can be affected by sleep”.
A doctor might recommend a sleep study to diagnose conditions like obstructive sleep apnea. This condition affects 1% to 4% of children but is more common – 20% to 70% – in children with obesity. For chronic insomnia, cognitive behavioral therapy (CBT) is often the most effective treatment.
Avoid giving supplements like melatonin without consulting a healthcare provider. These can cause side effects like morning grogginess. Keeping a sleep log that tracks patterns, hours slept, and disruptions can also provide helpful insights for your doctor.
Sleep as Part of Complete Mental Health Care
Why a Complete Care Approach Matters
Sleep plays a vital role in your child’s mental well-being, influencing everything from stress management to school performance. While earlier sections touched on how sleep issues can contribute to specific mental health conditions, addressing sleep in isolation often falls short. A well-rounded mental health plan weaves together sleep, nutrition, exercise, therapy, and family dynamics to achieve lasting results.
Better sleep can pave the way for improved emotional stability, sharper concentration, and stronger relationships. For instance, resolving a sleep disorder like obstructive sleep apnea has been shown, in some cases, to enhance attention and behavior so much that the need for psychiatric medications may be significantly reduced or re-evaluated. This underscores the importance of integrating sleep management into a broader treatment approach.
How Modyfi Health Addresses Sleep and Mental Health
Modyfi Health takes a comprehensive approach, creating personalized care plans that connect sleep with other essential aspects of health. During a 60-minute evaluation, their team examines symptoms alongside factors like sleep patterns, diet, exercise habits, and family interactions.
When sleep issues arise, they may recommend functional lab testing to uncover nutritional deficiencies, such as low iron levels, which can disrupt dopamine function and lead to restless sleep. Their care plans also include nutrition therapy to support melatonin production through Omega-3 supplementation, as well as exercise therapy to help regulate your child’s internal clock. For persistent sleep challenges, cognitive behavioral therapy (CBT) is offered. Known as the gold standard for insomnia treatment, CBT has also been shown to alleviate symptoms of depression and anxiety.
This approach acknowledges that sleep is shaped by a variety of factors. By addressing root causes, Modyfi Health provides sustainable solutions for improving both sleep and mental health.
Conclusion
In this guide, we’ve looked at how sleep impacts children’s emotional and behavioral health. Sleep is as crucial to their well-being as oxygen itself. As Rafael Pelayo from the Stanford Sleep Medicine Center aptly states:
“Your life is a reflection of how you sleep, and how you sleep is a reflection of your life”.
We’ve seen how sleep affects emotional regulation, behavior, and mental health. Poor sleep can lead to challenges like anxiety, depression, and ADHD symptoms, while these same conditions can further disrupt sleep – creating a vicious cycle. With nearly 80% of teenagers not getting enough sleep and 20–40% of school-age children struggling to fall or stay asleep, the need for action is urgent.
You can start making changes today. Simple steps like maintaining consistent bedtimes and wake times – even on weekends – can make a big difference. Research shows that establishing regular sleep routines early helps with emotional regulation and reduces impulsivity later in life. A 30-minute wind-down routine, keeping bedroom temperatures between 65–70°F, and setting a digital curfew are practical strategies that can lead to noticeable improvements. By incorporating these habits into your child’s care plan, you’re laying the groundwork for lasting benefits to their overall mental and emotional health.
Is Poor Sleep Fueling Your Child’s Emotional Struggles?
At Modyfi Health, we don’t look at sleep in a vacuum. We investigate the metabolic, nutritional, and emotional root causes behind sleep issues to build a personalized, lasting solution. Schedule a Comprehensive 60-Minute Evaluation for Your Child and discover the difference of whole-person care.
FAQs
How can I tell if my child’s sleep problem is affecting their mental health?
Signs that your child’s sleep problems might be affecting their mental health can include more frequent negative emotions, difficulty managing stress, or clear changes in behavior and mood. Sleep struggles are often connected to these challenges, making it important to focus on improving their sleep to support their overall well-being.
What’s the fastest bedtime routine change that actually helps kids sleep better?
Establishing a consistent and calming bedtime routine is one of the fastest ways to improve kids’ sleep. Simple activities like reading a book, singing a lullaby, or listening to soothing music for 20–30 minutes before bed can make a big difference in sleep quality. Another helpful strategy is using a limited number of “bedtime passes” to manage those late-night trips out of bed, which can encourage better behavior. The secret to quick results? Stick to the routine – consistency and predictability are everything.
When should I talk to a doctor about snoring, insomnia, or melatonin?
If your child continues to struggle with sleep or their sleep issues are impacting their overall well-being – like having consistent trouble falling or staying asleep, or experiencing loud snoring – it’s important to consult a doctor. A healthcare provider can assess for potential conditions such as sleep apnea. Additionally, if you’re thinking about using melatonin supplements, it’s crucial to talk with a doctor first to ensure they’re used safely, particularly for chronic or more serious sleep concerns.
